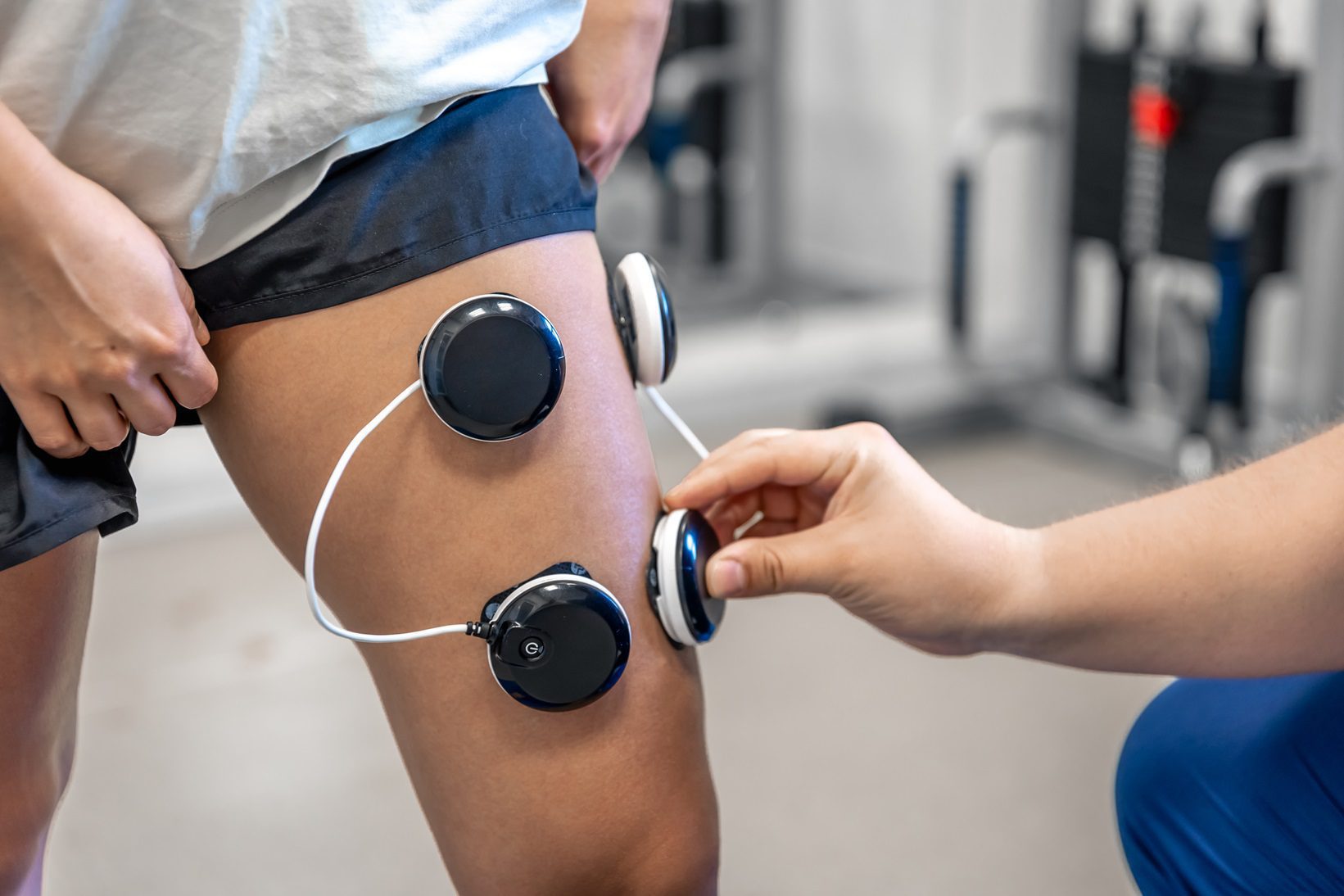
Spastic paraplegia is a neurological disorder characterized by progressive weakness and increased muscle tone in the lower limbs, affecting mobility and balance. This condition may arise from a variety of causes, ranging from genetic factors to diseases affecting the central nervous system, such as multiple sclerosis or spinal cord injuries. Spastic paraplegia can present with varying degrees of severity, and its symptoms significantly impact the quality of life of affected individuals.
What is Spastic Paraplegia?

Spastic paraplegia is a form of paralysis affecting the lower extremities caused by damage to the motor neurons that control the leg muscles. This condition is progressive and is primarily characterized by spasticity, defined as an increase in muscle tone that leads to stiffness and impaired movement. Spasticity may result in reduced motor control and muscle strength, making everyday activities such as walking, standing, or maintaining balance challenging.
There are different clinical forms of presentation of spastic paraplegia:
- Hereditary spastic paraplegia: A genetic disorder in which symptoms appear gradually and progress slowly, primarily affecting the muscles of the lower limbs.
- Acquired spastic paraplegia: This form may result from injuries, infections, or diseases that damage the neural pathways responsible for motor control.
Causes of Spastic Paraplegia
The causes of spastic paraplegia may vary and depend on whether the condition is hereditary or acquired. Some of the most common causes include:
- Genetic mutations: Hereditary spastic paraplegia is caused by mutations in various genes, leading to degeneration of neural pathways and impaired lower limb movement. More than 80 types of hereditary spastic paraplegia have been identified, each associated with different genetic mutations.
- Spinal cord injuries: Trauma to the spine, such as motor vehicle accidents or falls, can damage the spinal cord and lead to spastic paraplegia.
- Neurological disorders: Conditions such as multiple sclerosis, cerebral palsy, or neurodegenerative diseases may cause spasticity in the lower limbs, leading to spastic paraplegia.
- Infections or inflammation: Meningitis, encephalitis, and other inflammatory processes affecting the central nervous system may also lead to spasticity in the lower extremities.
Symptoms of Spastic Paraplegia
The symptoms of spastic paraplegia may vary depending on the underlying cause and the severity of the condition. Some of the most common symptoms include:
- Muscle stiffness and spasticity: The muscles of the lower limbs become rigid, making smooth and coordinated movements difficult.
- Lower limb weakness: Muscle strength in the legs is reduced, which may lead to difficulty standing or walking.
- Spastic gait: Individuals with spastic paraplegia may exhibit an abnormal gait pattern, characterized by dragging or scissoring of the legs due to increased muscle tone.
- Fatigue and muscle pain: Persistent stiffness and weakness may lead to fatigue and muscle discomfort in the lower limbs.
As the disease progresses, mobility becomes increasingly limited, which may lead to the need for walking aids or a wheelchair.
Diagnosis of Spastic Paraplegia
The diagnosis of spastic paraplegia involves a comprehensive medical evaluation to determine the underlying cause of the symptoms. Some of the tests and assessments that may be performed include:
- Neurological examination: A comprehensive assessment of muscle tone, strength, reflexes, and coordination helps identify spasticity and motor impairment.
- Imaging studies: Tests such as magnetic resonance imaging (MRI) or computed tomography (CT) scans allow visualization of any lesions or abnormalities in the spinal cord and brain.
- Genetic testing: In cases of hereditary spastic paraplegia, genetic analysis allows the identification of specific mutations in genes associated with this condition.
- Electromyography (EMG): This test measures the electrical activity of muscles and helps assess neuromuscular function, determining the degree of spasticity and impairment.
Treatment of Spastic Paraplegia
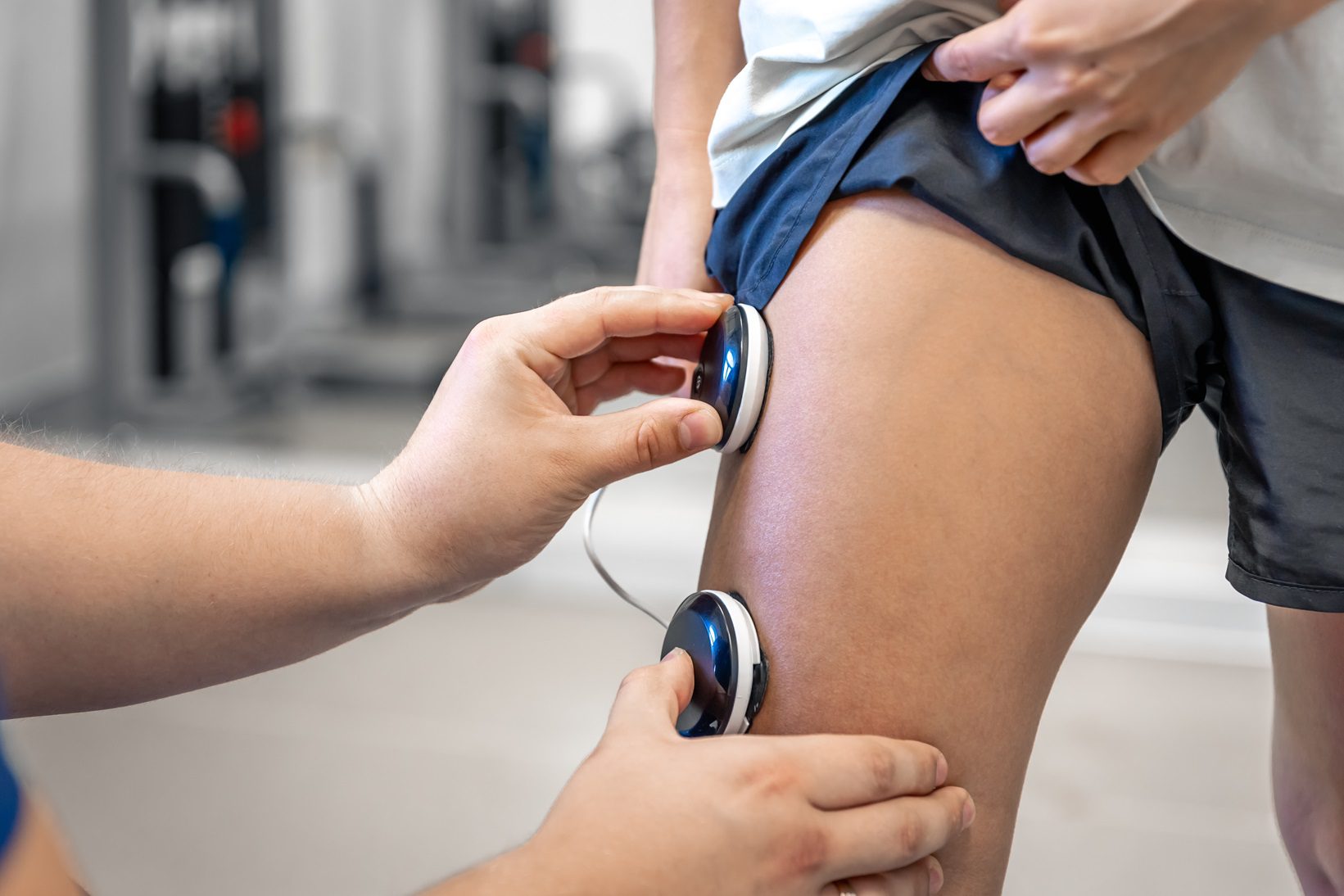
Currently, there is no cure for spastic paraplegia; however, several treatments may help alleviate symptoms and improve patients’ quality of life. Treatment options include:
- Physical therapy and rehabilitation: Physiotherapy exercises are essential to improve strength, flexibility, and coordination in the lower limbs. In addition, physiotherapists may provide stretching techniques to reduce muscle stiffness.
- Occupational therapy: This therapy helps patients perform daily activities more effectively by using assistive devices and adapting environments to facilitate mobility.
- Antispasmodic medications: Drugs such as baclofen or diazepam may help reduce spasticity and improve muscle control.
- Botulinum toxin (Botox): Injections of botulinum toxin may reduce spasticity in the lower limb muscles, providing temporary relief and improving mobility.
- Surgery: In severe cases where other treatments have not been effective, surgical intervention may be considered to reduce spasticity. This may include procedures such as selective rhizotomy, in which specific nerve roots responsible for spasticity are surgically severed.
Management and Quality of Life in Spastic Paraplegia
The management of spastic paraplegia requires a comprehensive approach that addresses the physical, emotional, and social needs of patients. Some recommendations to improve quality of life include:
- Regular exercise: Moderate physical activity is beneficial for reducing muscle stiffness and maintaining strength.
- Psychological counseling: Living with spastic paraplegia can be challenging, and psychological therapy may help patients cope with the emotional difficulties associated with the condition.
- Support network: Having a network of family, friends, and support groups can be a valuable resource for coping with daily challenges.
- Mobility aids: The use of devices such as canes, walkers, or wheelchairs facilitates mobility and enables patients to maintain independence.
A multidisciplinary approach involving physicians, physiotherapists, occupational therapists, and psychologists is essential to provide comprehensive care and improve patient well-being.
Conclusion
Spastic paraplegia is a condition that affects mobility and the quality of life of those who live with it. From its genetic causes to its acquired forms, this disorder is characterized by spasticity and weakness in the lower extremities, which impair movement and balance. Although there is no cure, early diagnosis and appropriate management can help alleviate symptoms and improve functional outcomes.
Medical interventions, together with physical therapy and psychological support, enable individuals with spastic paraplegia to cope with the challenges of the condition and achieve a better quality of life. With ongoing advances in research and therapeutic approaches, there is hope for the development of more effective treatments that allow for improved management of this condition.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields