
Apoplexy is a medical term that has historically been used to describe a sudden loss of neurological function, typically caused by a stroke. Although more specific terms such as stroke or cerebral hemorrhage are preferred כיום, the term apoplexy retains important clinical and semantic value, particularly in historical contexts and certain medical classifications.
Definition and Evolution of the Term
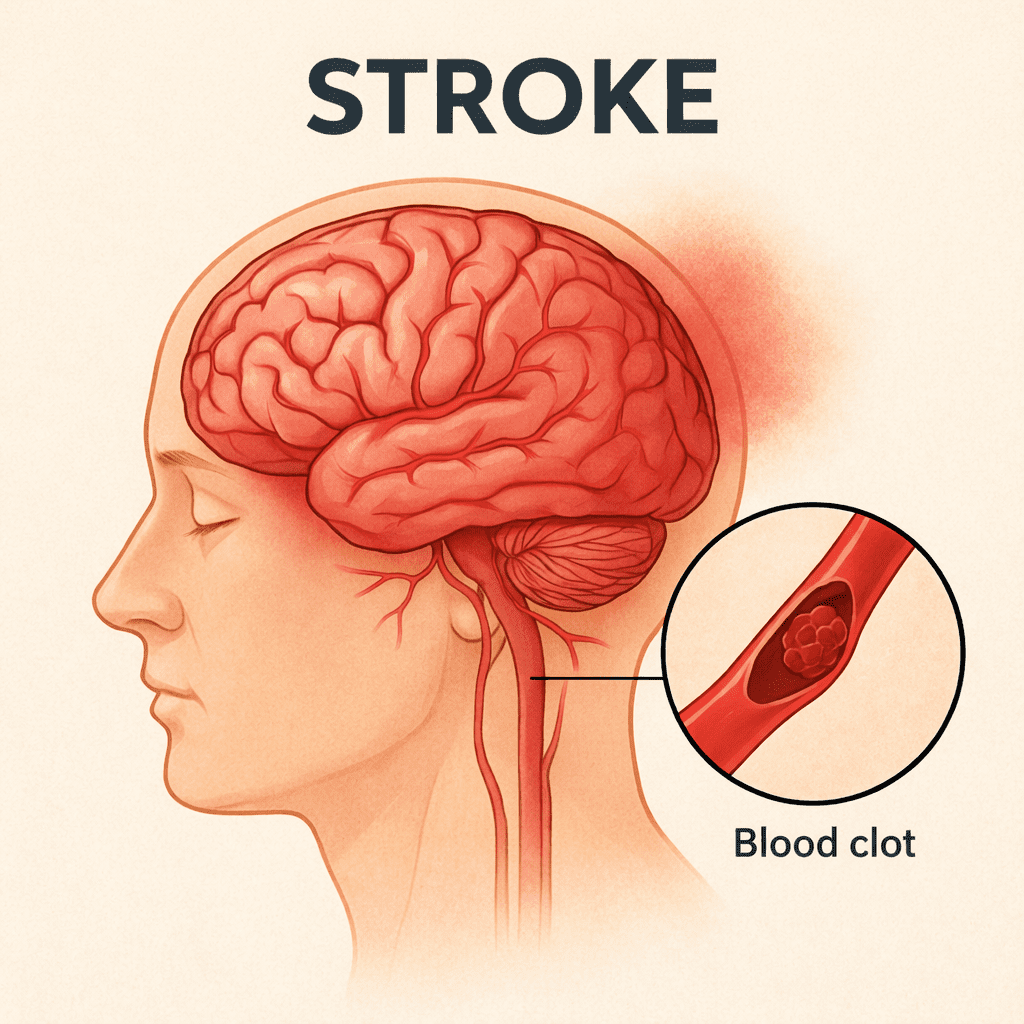
Originally, apoplexy was a broad category that encompassed any type of sudden collapse accompanied by loss of consciousness or mobility, caused by cerebral dysfunction. With advances in neurology and imaging techniques, it has become possible to differentiate between various causes, such as ischemic stroke, hemorrhagic stroke, epilepsy, and even certain brain tumors.
Nevertheless, in many older medical texts and even in common language, apoplexy is used as a synonym for a devastating neurological event, characterized by the sudden loss of motor or cognitive functions.
Modern Classification
Currently, apoplexy is primarily classified into two main types, according to the underlying cause:
-
Ischemic apoplexy: results from an interruption in cerebral blood flow, whether due to thrombosis, embolism, or systemic hypoperfusion. It accounts for 80–85% of all cases.
-
Hemorrhagic apoplexy: occurs when a cerebral blood vessel ruptures, leading to bleeding within the brain parenchyma or the meningeal spaces. This type is generally associated with a poorer immediate prognosis.
In both cases, the consequence is an acute dysfunction of neurons, either due to lack of oxygen or compression caused by bleeding.
Risk Factors
The risk factors associated with apoplexy are well established and, in most cases, modifiable. The most relevant include:
-
Arterial Hypertension
-
Diabetes Mellitus
-
Dyslipidemia
-
Smoking
-
Sedentary Lifestyle
-
Cardiac diseases such as atrial fibrillation
Advanced age also significantly increases the risk, as do a family history of cerebrovascular events. Early detection of these factors enables active prevention of apoplexy episodes.
Clinical Manifestations
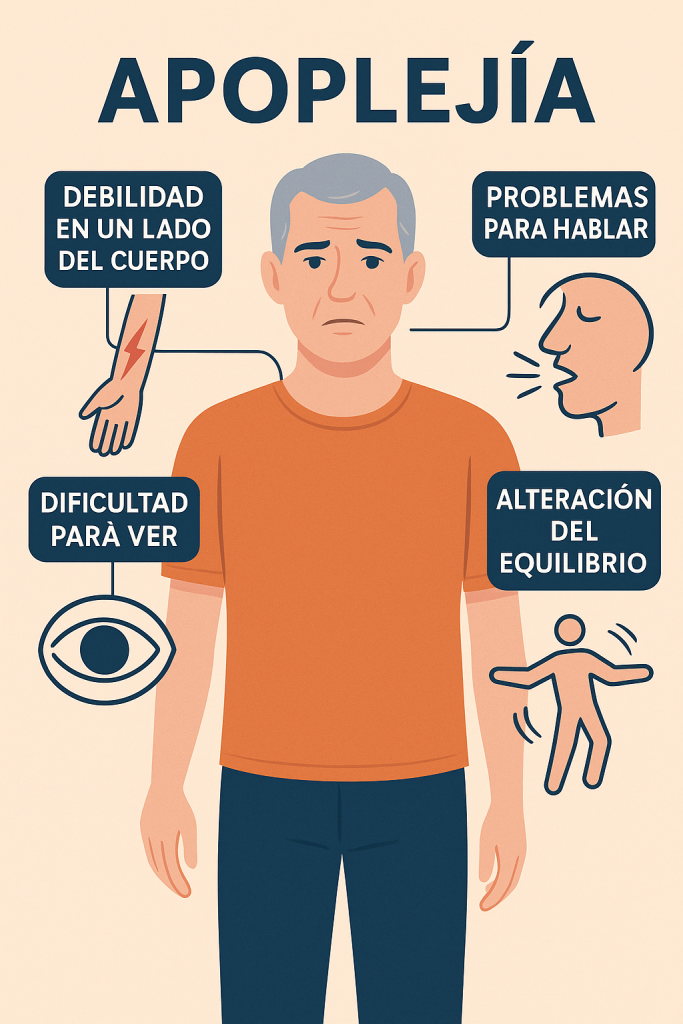
The signs and symptoms of apoplexy may vary depending on the affected brain territory, but generally include:
-
Sudden weakness or paralysis of one part of the body
-
Difficulty speaking or understanding language (aphasia)
-
Loss of vision in one or both eyes
-
Dizziness, loss of balance, or coordination
-
Sudden and severe headache, especially in hemorrhagic apoplexy
Early recognition of these symptoms is essential to activate emergency protocols and minimize brain damage.
Diagnosis
In suspected apoplexy, diagnosis must be immediate. The first step is to perform a cranial computed tomography (CT) scan to differentiate between an ischemic or hemorrhagic cause. This may be followed by additional studies such as magnetic resonance imaging (MRI), CT angiography, or carotid Doppler ultrasound.
Laboratory tests help rule out hypoglycemia, electrolyte imbalances, or infectious causes. An electrocardiogram and echocardiogram can identify cardiac sources, such as emboli of atrial origin.
The faster the diagnosis is made, the greater the chances of effective intervention in cases of apoplexy.
Treatment
The treatment of apoplexy varies depending on the type:
-
In ischemic apoplexy, if the patient arrives at the hospital within 4.5 hours from symptom onset, they may be eligible for intravenous thrombolysis (tPA). In some cases, mechanical thrombectomy can be performed to directly remove the clot.
-
In hemorrhagic apoplexy, management is more conservative and includes blood pressure control, measures to reduce intracranial pressure, and, in some cases, decompressive surgery or hematoma evacuation.
In both cases, a multidisciplinary approach is essential. This includes intensive care, physical rehabilitation, occupational therapy, and psychological support.
Prognosis and Complications
The prognosis of apoplexy depends on the size of the lesion, the affected brain territory, the speed at which treatment was initiated, and the patient’s pre-existing conditions. While some individuals recover almost completely, others may be left with permanent sequelae such as:
-
Hemiparesis
-
Speech disorders
-
Cognitive dysfunction
-
Emotional disturbances or post-stroke depression
In severe cases, especially in hemorrhagic apoplexy, brain death or fatality due to brainstem herniation may occur.
Prevention
The best strategy against apoplexy is primary prevention. Controlling risk factors, maintaining a balanced diet, engaging in regular physical activity, and avoiding tobacco and alcohol consumption are fundamental pillars.
Additionally, in high-risk patients, treatment with anticoagulants, antiplatelet agents, or statins may be indicated. Awareness campaigns such as the FAST acronym (Face, Arms, Speech, Time) have been key in improving early recognition of apoplexy symptoms.
Apoplexy in Medical History
Apoplexy has been a subject of study since ancient times. Hippocrates described it as a sudden collapse without fever or convulsions, and for centuries it was assumed to be a natural consequence of aging. It was not until the development of pathological anatomy and modern neurology that its true causes were understood.
Today, the term apoplexy persists as a reminder of the history of medicine and as a synonym for a severe cerebrovascular event in many languages and clinical traditions.
Rehabilitation
The rehabilitation process following apoplexy is prolonged and requires a comprehensive approach. Therapy should be initiated as early as possible, even during hospitalization. The main areas of intervention include:
-
Physiotherapy to improve mobility
-
Speech therapy to treat speech disorders
-
Occupational therapy to relearn activities of daily living
-
Psychological support and cognitive therapy
A well-planned rehabilitation program can make a significant difference in the patient’s future level of independence.
Conclusion
Apoplexy represents one of the most critical neurological emergencies a person can experience. Early recognition, immediate treatment, and effective prevention are essential elements to reduce its impact on patients’ quality of life.
Despite advances in modern medicine, apoplexy remains a clinical challenge due to its unpredictable and devastating nature. It is the responsibility of healthcare systems, medical professionals, and society as a whole to promote education, prevention, and equitable access to treatments that can save lives and minimize the long-term consequences of this condition.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields



