Spasticity is a disorder of muscle tone that frequently affects patients who have experienced a stroke, spinal cord injury, multiple sclerosis, or cerebral palsy. Assessing its severity in a reliable and systematic manner is a fundamental step in establishing appropriate treatment and monitoring its progression.
In this context, the Ashworth scale has become one of the most widely used clinical tools in neurological and rehabilitation practice. Its simplicity, applicability, and comparative value make it a valuable resource for both physiotherapists and physicians.
What is the Ashworth scale?

The Ashworth scale is a clinical assessment tool used to measure the degree of spasticity in a muscle or muscle group. It was developed in 1964 by Brian Ashworth, a researcher who sought a systematic method to evaluate increased muscle tone in patients with multiple sclerosis. Since then, its use has expanded to various neurological conditions and to both clinical and research settings.
Essentially, the Ashworth scale is based on the resistance a muscle offers during passive movement. In other words, the examiner moves the patient’s limb in a controlled manner and assesses the degree of stiffness or resistance encountered during the movement. Based on this observation, a score is assigned ranging from 0 to 4, where 0 indicates no spasticity and 4 indicates extreme rigidity that prevents movement.
How is the Ashworth scale applied?
The assessment procedure using the Ashworth scale is relatively straightforward, but it requires clinical experience to achieve accurate evaluation. The patient should be in a comfortable position, preferably lying down, with the muscles relaxed. The clinician passively moves the joint through its full range of motion, without any active participation from the patient.
The key lies in the speed of movement, as spasticity is a velocity-dependent phenomenon. The faster the muscle is moved, the greater the resistance tends to be if spasticity is present. Therefore, the examiner should apply a rapid movement, while ensuring it is safe and does not cause pain.
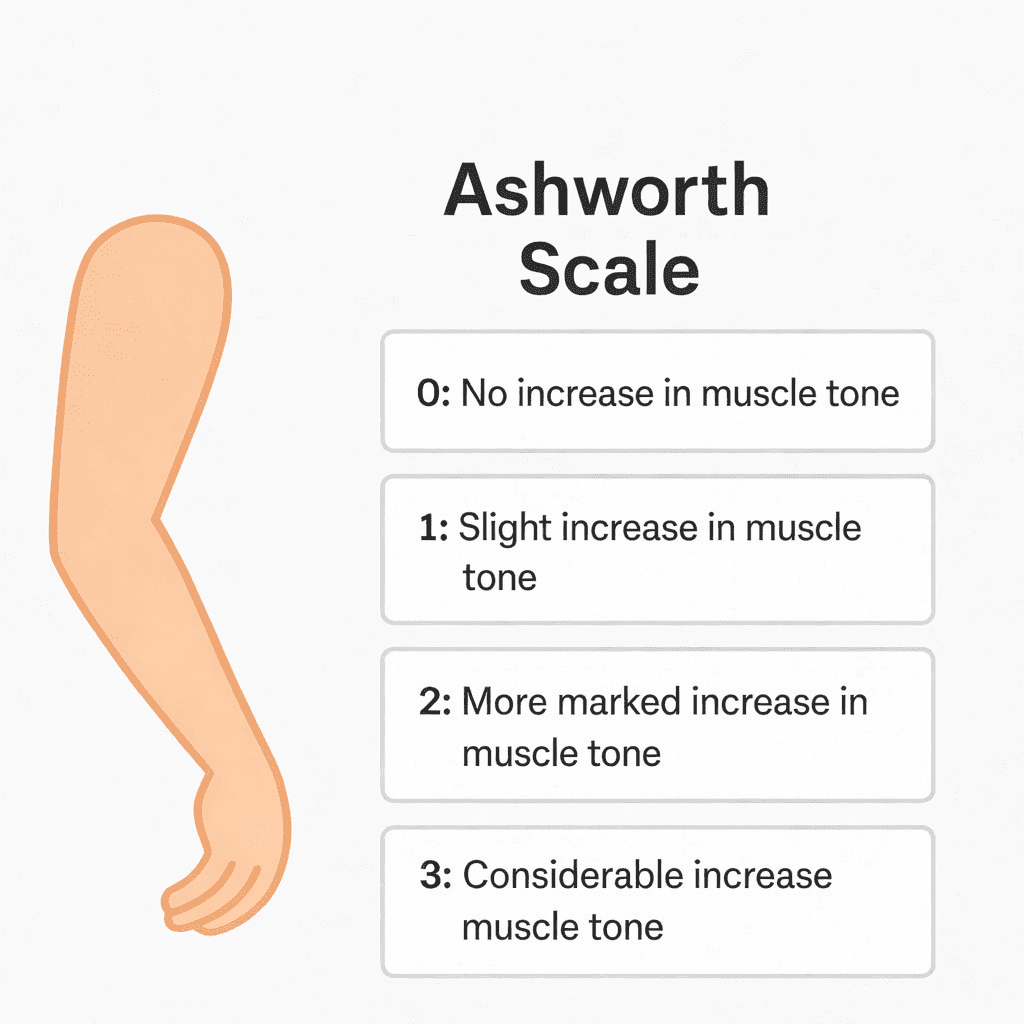
Once the movement has been performed, a score is assigned according to the following criteria of the original Ashworth scale:
0: Normal muscle tone
1: Slight increase in muscle tone, with minimal resistance at the end of the range of motion
2: More marked increase in muscle tone throughout the range of motion, but the limb moves easily
3: Considerable increase in muscle tone, making passive movement difficult
4: The affected part is rigid in flexion or extension
Limitations of the Ashworth Scale
Despite its widespread use, the Ashworth Scale presents limitations that must be taken into account. One of the main criticisms is its subjectivity. Because it relies exclusively on the evaluator’s perception, results may vary between different professionals, or even between assessments conducted by the same professional at different times.
In addition, the Ashworth Scale does not clearly distinguish between spasticity and other forms of hypertonia, such as extrapyramidal rigidity. It also does not adequately assess other factors that may influence muscle tone, such as pain, muscle contracture, or patient anxiety.
These limitations led to the development of a modified version, known as the Modified Ashworth Scale, which includes an intermediate score (1+) to improve sensitivity and better capture clinical nuances. Even so, both versions continue to be a subject of discussion among experts.
Clinical applications of the Ashworth Scale
Despite its limitations, the Ashworth Scale remains a valuable tool in various clinical contexts. Its main utility lies in the initial assessment and in the longitudinal follow-up of patients with neurological damage. It allows establishing a baseline for designing physiotherapy programs, selecting orthotic devices, or deciding on pharmacological interventions.
In patients receiving botulinum toxin treatment to control spasticity, for example, the Ashworth Scale is used before and after administration to assess its effectiveness. Similarly, it is used to document the response to physical therapies such as passive stretching, hydrotherapy, functional electrical stimulation, or motor control exercises.
It also plays a relevant role in clinical research. Numerous studies evaluating new techniques or pharmacological treatments aimed at reducing spasticity use the Ashworth Scale as an outcome measure due to its simplicity, reproducibility, and international recognition.
Comparison with other scales
There are other scales that are also used to assess muscle tone and spasticity, such as the Tardieu Scale. Unlike the Ashworth Scale, the Tardieu Scale takes into account not only resistance to movement, but also the speed of stretch and the occurrence of myotatic reflexes.
Another difference is that the Tardieu Scale requires identifying the angle at which resistance appears, which provides greater precision but also more complexity. For this reason, the Ashworth Scale continues to be preferred in settings where a rapid assessment is needed and angular measurement equipment is not available.
Both scales can complement each other. In some rehabilitation programs, the Ashworth Scale is used as an initial approach, and the Tardieu Scale for more detailed analysis.
Clinical staff training
Since the Ashworth Scale largely depends on the evaluator’s experience and sensitivity, it is essential that professionals receive proper training. Training in the correct application of the scale, together with supervised clinical practice, helps improve the reliability of assessments and reduces errors derived from subjectivity.
Multidisciplinary teams working in neurological rehabilitation should establish clear protocols for the use of this tool. Ideally, assessments should be performed by the same professional over time to improve data consistency. In addition, it is recommended to document the conditions under which the test was conducted, such as patient positioning or level of cooperation.
Future of the Ashworth Scale
With the advancement of technology, it is likely that in the future clinical tools such as the Ashworth Scale will be combined with objective technologies. Motion sensors, electromyography, and force platforms can provide complementary data to better quantify muscle tone and treatment response.
However, the practicality and low cost of the Ashworth Scale ensure that it will remain a fundamental tool, especially in settings where advanced technological equipment is not available.
In addition, its educational value is undeniable. Teaching the Ashworth Scale to physiotherapy and medical students helps introduce fundamental concepts of muscle tone, neurological control, and therapeutic planning, making it a highly useful teaching tool.
Conclusion
The Ashworth Scale represents an essential clinical tool for assessing muscle spasticity in patients with neurological conditions. Although it is not without criticism, its simplicity, accessibility, and usefulness maintain it as a reference in the daily practice of physiotherapists and rehabilitation physicians. Understanding its advantages and limitations allows for maximizing its potential and appropriately integrating it into the comprehensive management of the neurological patient. The correct application of the Ashworth Scale, combined with other diagnostic and therapeutic strategies, can make a significant difference in the process of functional recovery and quality of life for individuals living with spasticity.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields