Cerebral oxygen deprivation, medically known as cerebral hypoxia, is a critical condition that can have devastating effects on neurological health. The human brain depends on oxygen to function properly. Even a brief interruption in oxygen supply can result in irreversible brain damage.
What is lack of oxygen in the brain?
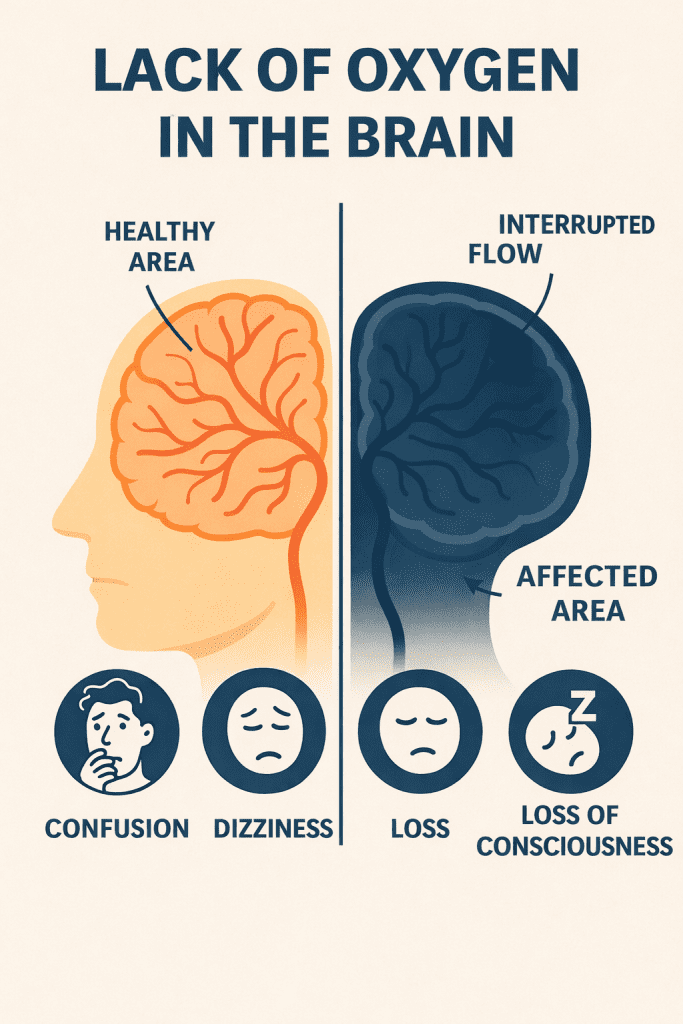
Lack of oxygen in the brain occurs when brain tissue does not receive sufficient oxygen to maintain its basic metabolic functions. It can be classified into several levels depending on its severity:
-
Mild cerebral hypoxia: partial reduction in oxygen supply.
-
Moderate cerebral hypoxia: significant, but not complete, reduction in oxygen supply.
-
Cerebral anoxia: complete interruption of oxygen supply.
These conditions directly impair the ability of neurons to generate energy, which may result in cell death, cerebral inflammation, and loss of cognitive or motor functions.
Causes of lack of oxygen in the brain
There are multiple potential causes of lack of oxygen in the brain. Some of the most common include:
-
Cardiac arrest: cessation of cardiac activity prevents oxygen from reaching the brain.
-
Stroke: may block blood flow to a region of the brain.
-
Asphyxia: due to airway obstruction or drowning.
-
Severe sleep apnea: repeated episodes of breathing interruption during sleep.
-
Traumatic brain injury: injuries that impair cerebral oxygenation.
-
Carbon monoxide poisoning: prevents hemoglobin from transporting oxygen.
-
Severe anemia: reduced capacity of the blood to transport oxygen.
-
Extreme altitudes: low levels of oxygen in the air.
Lack of oxygen in the brain may also occur during childbirth, which can lead to cerebral palsy or other developmental disorders if not treated promptly.
Symptoms of lack of oxygen in the brain
Symptoms vary depending on the duration and severity of the hypoxic episode. Some early and common signs include:
-
Dizziness and confusion.
-
Loss of coordination and balance.
-
Blurred or double vision.
-
Sudden headache.
-
Difficulty speaking or understanding.
-
Feeling of impending fainting.
In more severe cases, lack of oxygen in the brain may lead to:
-
Seizures.
-
Coma.
-
Permanent memory loss.
-
Limb paralysis.
-
Brain death.
These symptoms require immediate medical attention, as brain damage can progress rapidly if oxygen supply is not restored.
Neurological consequences of lack of oxygen in the brain
Lack of oxygen in the brain can lead to long-term sequelae, even if the acute episode is resolved. Among the most common consequences are:
-
Cognitive impairment: loss of abilities such as language, concentration, and memory.
-
Motor disorders: difficulty walking, tremors, or spasticity.
-
Emotional disturbances: depression, anxiety, or personality changes.
-
Post-hypoxic epilepsy: occurrence of recurrent seizures following the episode.
-
Immobility syndrome or persistent vegetative state in severe cases.
Prognosis depends on the duration of cerebral oxygen deprivation, the patient’s age, pre-existing conditions, and how quickly emergency treatment is initiated.
Diagnosis of cerebral hypoxia
To diagnose lack of oxygen in the brain, clinicians typically use a combination of tools:
-
Clinical assessment: evaluation of neurological signs and level of consciousness.
-
Computed tomography (CT scan): allows detection of structural brain damage.
-
Magnetic resonance imaging (MRI): more precise for evaluating soft tissues.
-
Electroencephalogram (EEG): measures the electrical activity of the brain.
-
Arterial blood gas analysis: assesses oxygen levels in the blood.
Additionally, specific biomarkers may be used to assess the severity of neuronal damage.
Treatment of lack of oxygen in the brain
The treatment aims to restore oxygen supply as early as possible and to limit neurological damage:
-
Oxygen therapy: supplemental oxygen is administered via mask or mechanical ventilation.
-
Cardiopulmonary resuscitation (CPR): essential in cases of cardiac arrest.
-
Induction of therapeutic hypothermia: reduces inflammation and protects neurons.
-
Intracranial pressure control: to prevent cerebral edema.
-
Pharmacological therapies: anticonvulsants, anticoagulants, or anti-inflammatory agents depending on the clinical context.
Subsequently, neurological rehabilitation is required, including physiotherapy, occupational therapy, speech therapy, and psychological support.
Prevention: how to avoid cerebral hypoxia
Preventing cerebral hypoxia involves controlling risk factors and acting promptly at the earliest signs:
-
Maintain good cardiovascular health.
-
Control conditions such as hypertension, diabetes, or sleep apnea.
-
Avoid environments with a risk of intoxication such as smoke or carbon monoxide exposure.
-
Use safety measures to prevent traumatic brain injury.
-
Do not delay medical attention in the presence of stroke symptoms.
In neonatology, labor monitoring and the use of resuscitation techniques are key to preventing hypoxic injury in the newborn.
Special cases: cerebral hypoxia in athletes and mountaineers
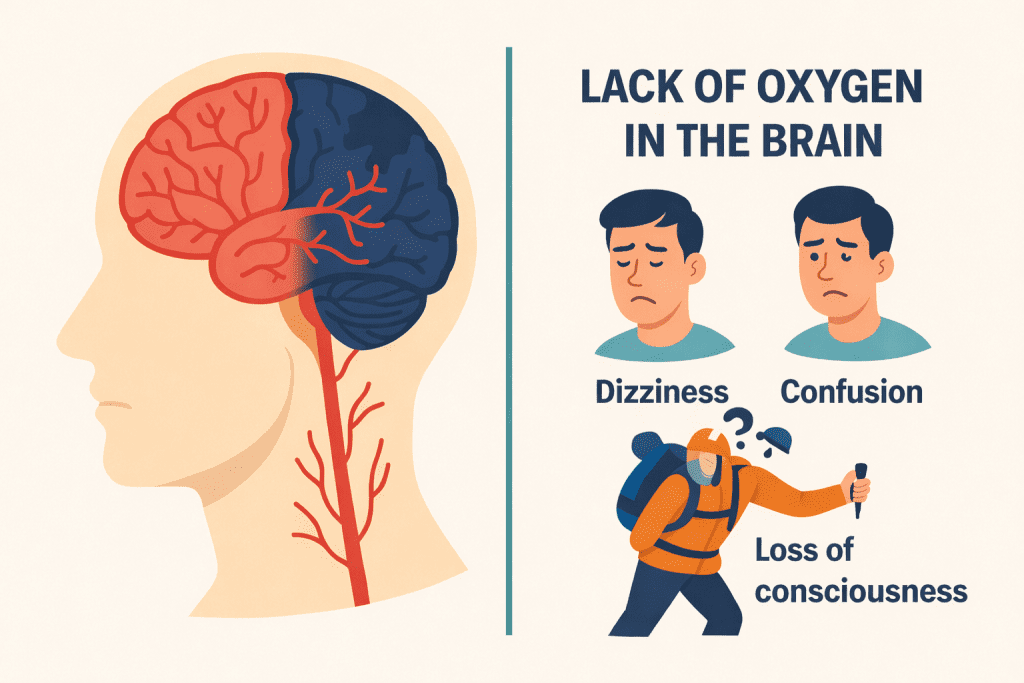
Some cases of cerebral hypoxia occur in non-clinical settings. High-altitude mountaineers and extreme athletes are particularly vulnerable:
-
At high altitudes above 2,500 meters, the partial pressure of oxygen decreases, which may lead to altitude sickness or high-altitude cerebral edema.
-
In sports such as apnea or free diving, voluntary hypoxia may occur, carrying significant risks if not properly trained.
These examples illustrate that cerebral hypoxia is not exclusive to pathological conditions, but can also affect healthy individuals in extreme situations.
Future research and neuroprotection
Neuroscience is focusing efforts on better understanding the mechanisms of hypoxia-induced neuronal injury. Current lines of research include:
-
Use of stem cells to regenerate damaged neurons.
-
Neuroprotective agents that block the post-hypoxic inflammatory cascade.
-
Gene therapies to enhance cerebral resilience to oxidative stress.
These strategies may offer hope to thousands of individuals affected by cerebral hypoxia each year.
Conclusion
Cerebral hypoxia is a serious medical condition that can lead to irreversible consequences within minutes. Its causes range from cardiac events to accidents or respiratory disorders, reflecting a broad spectrum of potential triggers. Early recognition of symptoms, rapid intervention, and a strong focus on prevention are essential to minimize the impact of this silent threat. With current medical advances and a commitment to a healthy lifestyle, it is possible to significantly reduce the risks associated with cerebral hypoxia.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields