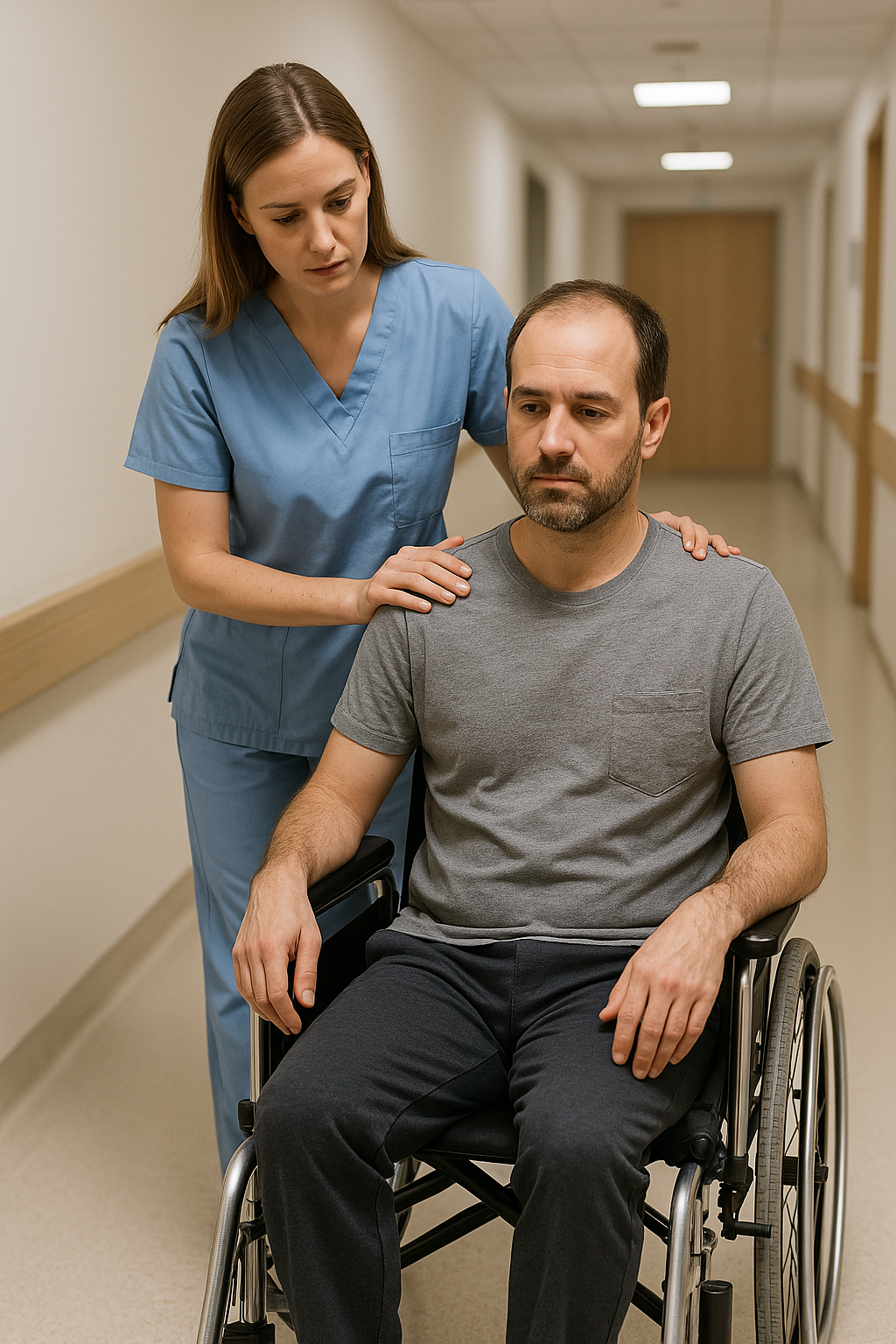
In the field of neurology, the terms plegia and paresis are essential for describing different degrees of motor impairment. Although they are often used interchangeably in common language, they refer to very different conditions in terms of severity, prognosis, and treatment.
What is paresis?

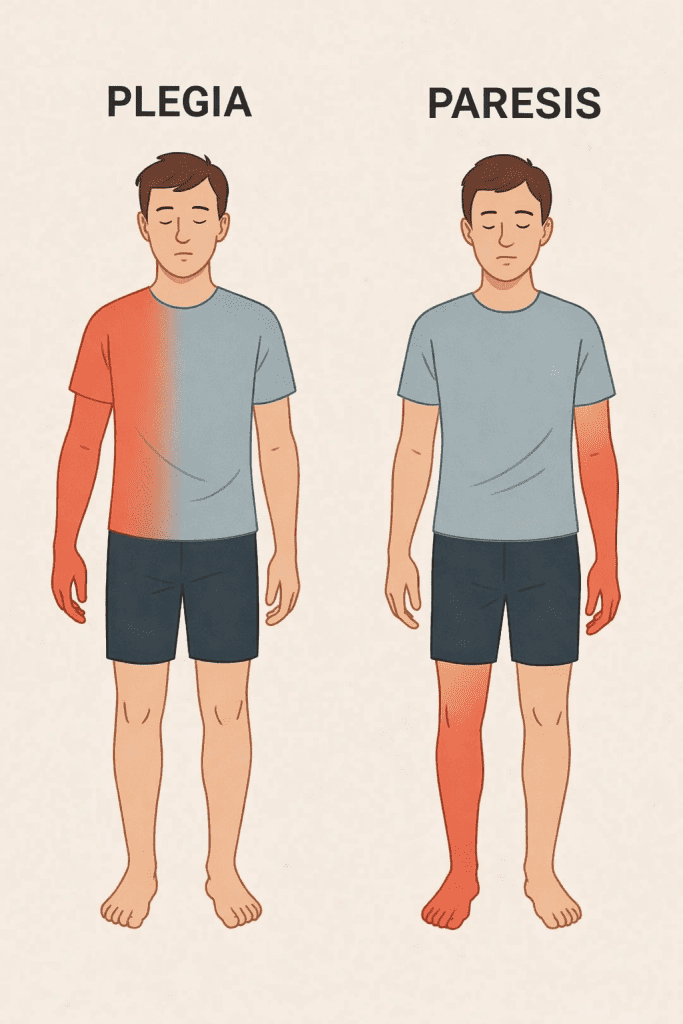
Paresis is defined as a partial weakness of voluntary muscles. It does not imply a complete loss of movement, but rather a significant reduction in strength or control over one or more limbs. There are several types of paresis, such as hemiparesis (one side of the body), paraparesis (both legs), monoparesis (one limb), and quadriparesis (all four limbs).
Common causes of paresis
- Stroke
- Partial spinal cord injuries
- Multiple sclerosis
- Brain or spinal tumors
- Nervous system infections
- Cerebral palsy
Symptoms of paresis
- Localized muscle weakness
- Reduced reflexes
- Muscle fatigue
- Difficulty walking or holding objects
What is plegia?
Plegia, or paralysis, is the complete loss of voluntary movement in one or more parts of the body. Unlike paresis, there is no residual capacity for movement. Plegia can affect different areas of the body and is also classified into types: hemiplegia (one side of the body), paraplegia (both legs), monoplegia (one limb), and quadriplegia (all four limbs).
Common causes of plegia
- Complete spinal cord injuries
- Severe strokes affecting extensive motor regions
- Traumatic brain injury
- Advanced neuromuscular diseases
Symptoms of plegia
- Complete absence of voluntary movement
- Loss of reflexes or hyperreflexia
- Muscle atrophy over time
- Dependence on mobility devices
Key differences between plegia and paresis
| Characteristic | Paresis | Plegia |
|---|---|---|
| Degree of movement | Partial | Absent |
| Prognosis | Better functional recovery | Depends on the type and extent of damage |
| Rehabilitation | More effective with continuous therapy | Requires more intensive assistance |
| Common example | Hemiparesis following a mild stroke | Quadriplegia due to severe spinal cord injury |
Understanding these differences is essential for accurate diagnosis and appropriate treatment.
Diagnosis and evaluation
The diagnosis of both plegia and paresis requires a detailed clinical evaluation. Neurologists perform assessments of muscle strength, coordination, reflexes, and sensation. Complementary studies such as magnetic resonance imaging, computed tomography scans, and electromyography are essential to identify the underlying cause.
Treatment and rehabilitation
Treatment of paresis
- Physiotherapy focused on strengthening weakened muscles
- Occupational therapy for activities of daily living
- Anti-inflammatory or neuromodulatory medication (depending on the underlying cause)
- Coordination and mobility exercises
Treatment of plegia
- Orthopedic and mobility devices (wheelchairs, braces)
- Intensive neurorehabilitation therapy
- Functional electrical stimulation
- Psychological and emotional support
Technology applied in rehabilitation
Advances in technology have significantly improved the quality of life of individuals with plegia and paresis. Tools such as robotic exoskeletons, virtual reality, and transcranial magnetic stimulation are transforming neurological treatment.
Patients with paresis particularly benefit from systems that promote repetitive movement, which facilitates neuroplasticity. In contrast, in patients with plegia, these technologies can help maintain muscle tone and prevent secondary complications such as joint stiffness.
Both plegia and paresis have a profound emotional impact on patients and their families. Feelings of frustration, loss of independence, and anxiety are common. Psychological support, social integration, and access to support networks are essential to improve overall well-being.
Prevention of complications
In both cases, it is essential to prevent associated complications such as:
- Pressure ulcers
- Muscle contractures
- Urinary tract infections (in cases of immobility)
- Depression and social isolation
This is achieved through multidisciplinary interventions and continuous medical follow-up.
Conclusion
The difference between plegia and paresis goes far beyond a semantic distinction; it has significant clinical and functional implications. Accurately identifying each condition allows for the development of more personalized and effective intervention strategies.
While paresis offers better prospects for recovery, plegia requires an approach focused on adaptation and compensation. In both cases, early access to rehabilitation programs and comprehensive support can make a significant difference in patients’ quality of life.
With advances in medical science and technology, the future appears promising for those facing motor impairments. Education, support, and rehabilitation are fundamental pillars in the recovery process, regardless of whether it involves mild paresis or complex plegia.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields