
In the therapeutic management of patients with neurological damage, the accurate assessment of spasticity is an essential part of the diagnostic and follow-up process.
In this context, the Tardieu Scale represents a highly valued alternative due to its ability to differentiate between different forms of hypertonia and to provide more detailed information than other conventional tools. Its use is increasingly widespread in clinical settings, especially in neurological physiotherapy, pediatric neurology, and motor rehabilitation.
What is the Tardieu Scale
The Tardieu Scale is a clinical system for assessing spastic muscle tone, based on the observation of the muscle’s response to stretches performed at different velocities. Unlike other scales such as the Ashworth Scale, which primarily focus on resistance to passive movement, the Tardieu Scale incorporates an angular and temporal dimension that improves the objectivity of the clinical assessment.
Originally developed by the French neurologist Gaston Tardieu, this tool assesses not only the magnitude of spasticity but also the point within the range of motion at which the abnormal muscle reaction appears. Thanks to this methodology, the Tardieu Scale allows differentiation between structural contracture and pure spasticity, which is key for defining treatments such as botulinum toxin administration, orthotic use, or the prescription of specific exercises.
How the Tardieu Scale is applied
The clinical procedure using the Tardieu Scale begins with proper patient positioning. The patient is generally placed in a relaxed and stable position, either in supine or seated posture depending on the joint being assessed. The examiner passively moves the muscle under three different velocity conditions:
V1: slow movement, as in a passive joint examination
V2: intermediate velocity, similar to the free fall of the limb segment without resistance
V3: fast movement, to elicit a maximal stretch response
At each of these velocities, the examiner observes two key elements: the angle at which resistance appears, known as R1, and the full passive range of motion, known as R2. The difference between R2 and R1 provides an indication of the dynamic component of spasticity.
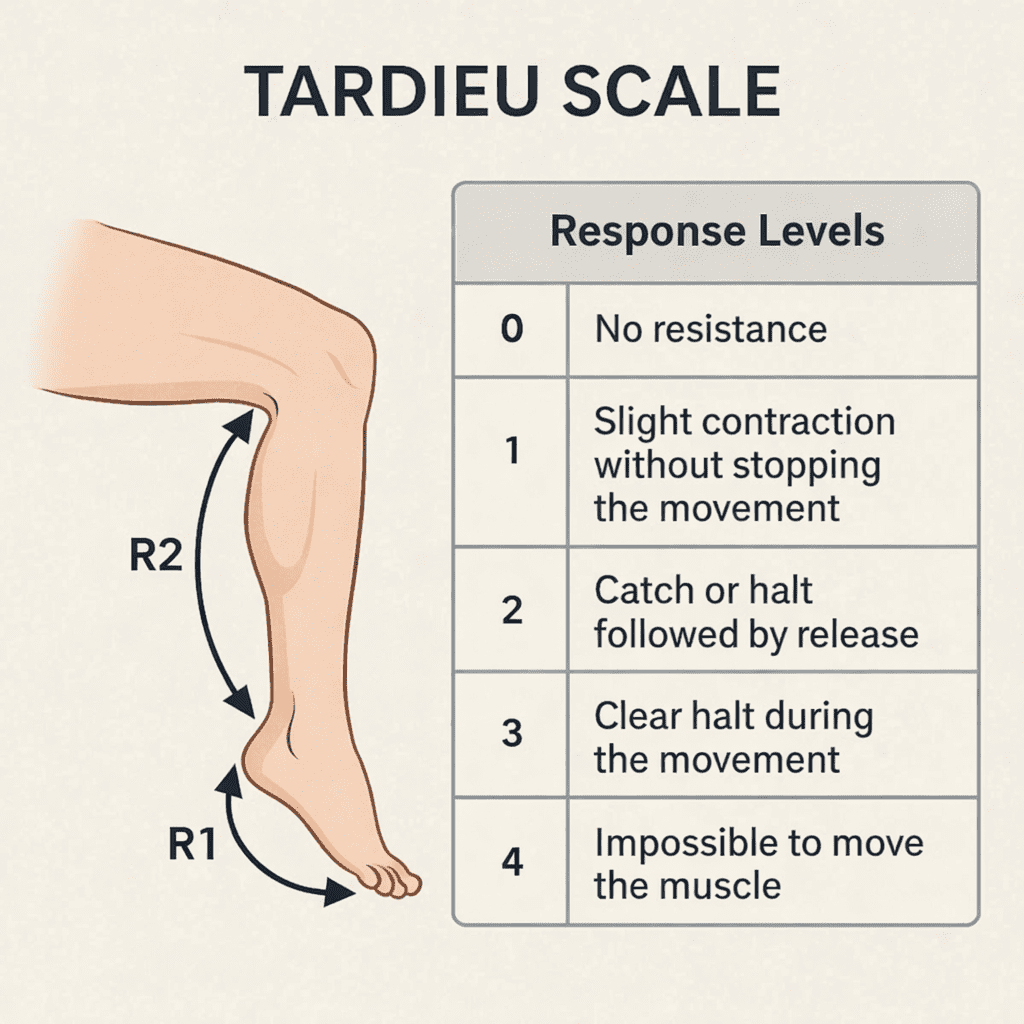 In addition, the muscle response is classified on an ordinal scale ranging from 0 to 4, where:
In addition, the muscle response is classified on an ordinal scale ranging from 0 to 4, where:
0 indicates that there is no resistance
1 indicates a slight contraction without interruption of movement
2 indicates a catch or stop followed by release
3 indicates a clear stop during movement
4 indicates that the muscle is impossible to move
This combination of angular values and qualitative ratings makes the Tardieu scale provide a more detailed assessment than other simpler scales.
Differences between the Tardieu scale and the Ashworth scale
Both the Tardieu scale and the Ashworth scale are widely used in the field of rehabilitation, but they are based on different principles. While the Ashworth scale focuses on the general resistance to passive movement, regardless of speed, the Tardieu scale emphasizes the speed of stretch and the exact point at which the reflex response occurs.
This allows the Tardieu scale to differentiate between spasticity and rigidity, something that is not possible with the Ashworth scale. Additionally, the angular measurement of the Tardieu scale enables a better quantification of treatment effectiveness over time, which is essential for making clinical decisions based on objective data.
Although the Ashworth scale is quicker and easier to apply, the Tardieu scale provides a richer assessment, especially useful in pediatric patients or in complex cases of cerebral palsy or multiple sclerosis.
Clinical indications for the use of the Tardieu scale
The Tardieu scale is particularly useful in the assessment of children with cerebral palsy, as it allows differentiation between spasticity and fixed musculoskeletal deformities. It is also used in adult patients with spinal cord injury, traumatic brain injury, or cerebrovascular events.
Additionally, it is routinely used in follow-up programs for patients receiving botulinum toxin as a treatment for spasticity. Comparing the R1 and R2 measurements before and after treatment allows objective visualization of the reduction in the spastic component and helps adjust the dose or target muscle in future applications.
In the surgical context, it is also used to determine when a contracture requires orthopedic intervention rather than conservative treatment. In this way, the Tardieu scale contributes to complex medical decisions based on objective data.
Advantages of the Tardieu scale
Among the main advantages of the Tardieu scale is its ability to reflect the reflex component of spasticity, that is, the muscle reaction that depends on the speed of movement. This allows for a more precise distinction between pure spasticity and other types of hypertonia.
Additionally, its angular approach facilitates the monitoring of therapeutic progress, which is useful for both physiotherapists and rehabilitation physicians. It also offers the possibility of identifying true muscle contractures, which require surgical approaches or the use of static splints.
Another advantage is its applicability across different body segments, as it can be used in the upper limbs, lower limbs, and even the trunk, adapting the method to the function of each muscle group.
Disadvantages and limitations

Despite its multiple benefits, the Tardieu scale also has limitations. The main one is that it requires greater technical training and practical experience from the evaluator. The precise identification of the R1 and R2 angles may vary between professionals, which introduces a certain degree of subjectivity.
Additionally, a goniometer is required to accurately measure joint angles, which implies a slight additional time investment. In settings with a high clinical workload, this can represent a practical barrier to its routine use.
However, with proper training and standardized protocols, these barriers can be easily overcome, and the benefits of the Tardieu scale ultimately outweigh the initial effort required.
Implementation in clinical teams
Effective implementation of the Tardieu scale in rehabilitation centers requires structured training. It is recommended that professionals perform supervised practice to improve inter-rater reliability and establish common interpretation criteria.
The systematic use of this scale within multidisciplinary teams allows for more consistent and objective decision-making. It also supports clear documentation in medical records and the preparation of reports for follow-up or referral.
Additionally, its use supports clinical research, as its results can be quantified and statistically analyzed in studies on new treatments, orthopedic devices, or advanced physiotherapy programs.
Conclusion
The Tardieu scale has established itself as a precise and detailed assessment tool for evaluating spasticity in patients with neurological damage. Its methodology, based on movement velocity and angular measurement, allows differentiation between types of hypertonia, detection of contractures, and objective evaluation of treatment response.
Although it requires more technical training than other scales, its clinical value is undeniable. The Tardieu scale not only improves functional diagnosis but also optimizes therapeutic planning and patient progression. For all these reasons, it represents a valuable ally in modern clinical practice, and its continued adoption is helping to raise the standard of care in neurological rehabilitation.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields



