
Achalasia is a rare esophageal disorder that impairs the body’s ability to transport food into the stomach. It is primarily characterized by the failure of the lower esophageal sphincter (LES) to relax properly during swallowing, leading to dysphagia, food regurgitation, and, in some cases, chest pain or weight loss. Although it is a chronic condition, effective treatments are currently available that can significantly improve patients’ quality of life.
What is achalasia?
Achalasia is a primary esophageal motility disorder that disrupts normal esophageal function. Under normal conditions, the esophagus uses coordinated rhythmic muscular contractions, known as peristalsis, to propel food toward the stomach. In achalasia, this activity is impaired: the esophageal body loses the ability to generate effective peristalsis, and the lower esophageal sphincter fails to relax appropriately during swallowing.
This results in a functional obstruction to the passage of food and liquids into the stomach, causing them to accumulate in the esophagus and, over time, leading to dilation of its walls.
Causes of achalasia
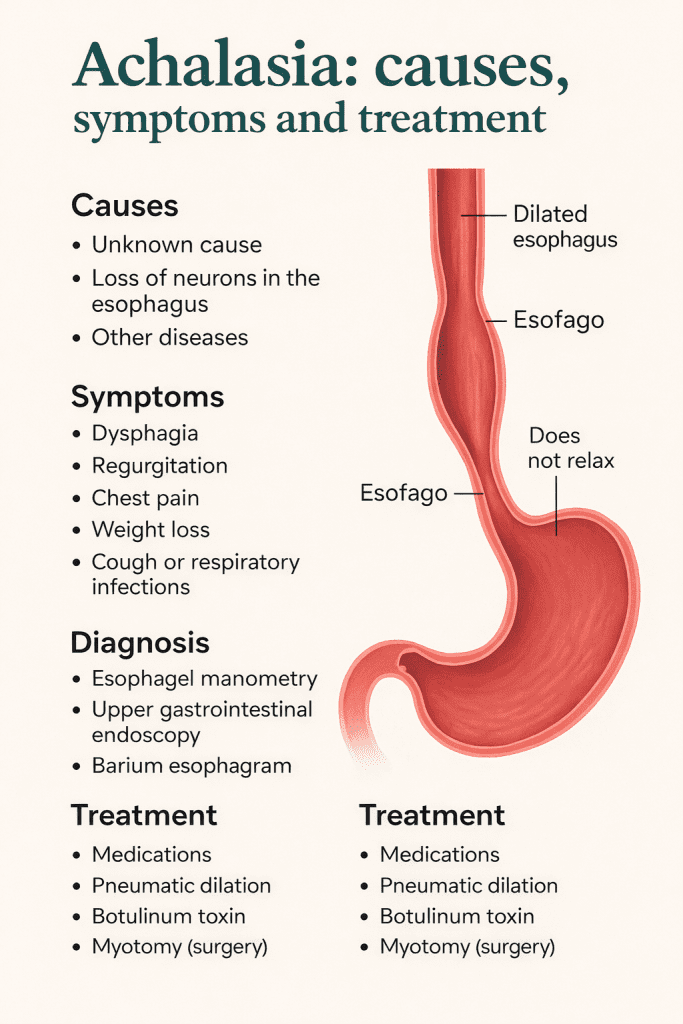
The exact cause of achalasia is not yet fully understood, but it is believed to be a degenerative process affecting the neurons of the myenteric plexus, also known as Auerbach’s plexus, which regulates esophageal muscle contractions. Some theories suggest an autoimmune or viral origin, although there is no complete consensus.
In rare cases, achalasia may be secondary to other conditions, such as esophageal or gastric cancer involving the lower esophageal sphincter, or infectious diseases such as Chagas disease, caused by the parasite Trypanosoma cruzi, which primarily affects individuals in Latin America.
Symptoms of achalasia
Symptoms of achalasia typically develop gradually and may be mistaken for other gastrointestinal conditions. The main symptoms include:
-
Dysphagia: difficulty swallowing solid foods, liquids, or both. It typically begins with solids and may progress to liquids.
-
Regurgitation: return of undigested food, particularly at night or when bending over.
-
Chest pain: typically pressure-like in nature and may be mistaken for cardiac pain.
-
Weight loss: due to difficulty maintaining adequate nutritional intake.
-
Chronic cough or respiratory infections: caused by aspiration of regurgitated contents into the lungs.
-
Retrosternal fullness or a sensation of chest pressure.
Diagnosis of achalasia
The diagnosis of achalasia requires a combination of clinical and instrumental tests:
1. Esophageal manometry
It is the most important test to confirm achalasia. It measures esophageal pressures and the pattern of contraction. Typical findings include absence of peristalsis and failure of the lower esophageal sphincter to relax. High-resolution manometry is currently preferred, as it allows classification of achalasia into three subtypes (I, II, and III), which helps guide the most appropriate treatment.
2. Upper gastrointestinal endoscopy
It is performed to rule out other causes of mechanical obstruction, such as tumors or strictures. In achalasia, a dilated esophagus is typically observed, with retained food and a distal sphincter that offers resistance to passage.
3. Barium esophagram
It consists of a radiographic study performed after ingestion of a contrast medium. It typically shows the characteristic “bird’s beak” appearance at the esophagogastric junction and allows assessment of esophageal dilation.
Treatment of achalasia
Although there is no definitive cure, the treatment of achalasia aims to relieve symptoms by facilitating the passage of food into the stomach. Available options include:
1. Pharmacological treatment
It has limited utility and is generally reserved for patients who are not candidates for invasive procedures.
-
Nitrates and calcium channel blockers: they reduce lower esophageal sphincter pressure, but their efficacy is modest and they may cause side effects such as hypotension or headaches.
2. Botulinum toxin (Botox)
It is injected directly into the lower esophageal sphincter via endoscopy. It induces temporary muscle relaxation and symptom relief. Its effect is time-limited, typically lasting 3 to 6 months, and may decrease in efficacy with repeated administrations.
3. Pneumatic dilation
It is performed by introducing a balloon into the lower esophageal sphincter, which is then inflated with air to disrupt the muscle fibers. It is an effective treatment, particularly in type II achalasia, although it carries a risk of perforation (approximately 2–5%).
4. Heller myotomy (surgery)
It is a surgical procedure that involves cutting the muscle fibers of the lower esophageal sphincter to allow its opening. It is performed laparoscopically and is usually combined with a partial fundoplication to prevent postoperative gastroesophageal reflux. It provides excellent long-term outcomes.
5. Peroral endoscopic myotomy (POEM)
It is a more recent, minimally invasive technique performed endoscopically. It allows division of the muscle from within the esophagus. It is effective across all achalasia subtypes, including more complex forms such as type III.
Complications
Untreated achalasia may lead to significant complications:
-
Severe esophageal dilation: leading to loss of esophageal motor function (sigmoid esophagus).
-
Malnutrition and significant weight loss.
-
Risk of pulmonary aspiration and pneumonia.
-
Increased risk of esophageal cancer (squamous cell carcinoma) over time.
Therefore, regular medical follow-up is essential in diagnosed patients.
Prognosis
With appropriate treatment, most patients experience significant symptom improvement and are able to lead a normal life. However, as it is a chronic condition, repeated interventions or long-term follow-up may be required. Prognosis depends in part on the achalasia subtype, the patient’s age, and the initial response to treatment.
Differences between achalasia and other esophageal diseases
It is important to differentiate achalasia from other causes of dysphagia or chest pain, such as:
-
Peptic esophageal stricture (due to gastroesophageal reflux)
-
Diffuse esophageal spasm
-
Systemic sclerosis
-
Esophageal tumors
An accurate diagnosis allows for the implementation of the most effective treatment and helps prevent complications.
Conclusion
Achalasia is an esophageal disorder that, although rare, can significantly impact a patient’s quality of life. Advances in diagnostic and therapeutic techniques have made it possible to provide highly effective, personalized solutions, even in complex cases. In the presence of symptoms such as persistent dysphagia, regurgitation, or unexplained chest pain, it is essential to seek medical evaluation to rule out achalasia or other esophageal disorders. Early and appropriate treatment can prevent complications and restore normal, symptom-free eating.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields


