Hyperparathyroidism is a condition in which the parathyroid glands, located in the neck, produce an excessive amount of parathyroid hormone (PTH). This hormone is responsible for regulating calcium and phosphorus levels in the body. When PTH is elevated, blood calcium levels increase, which can lead to a range of health complications, including an increased risk of cardiovascular disease and stroke. The connection between hyperparathyroidism and stroke is not always immediately apparent, but understanding it is essential for preventing serious complications.
What is Hyperparathyroidism?
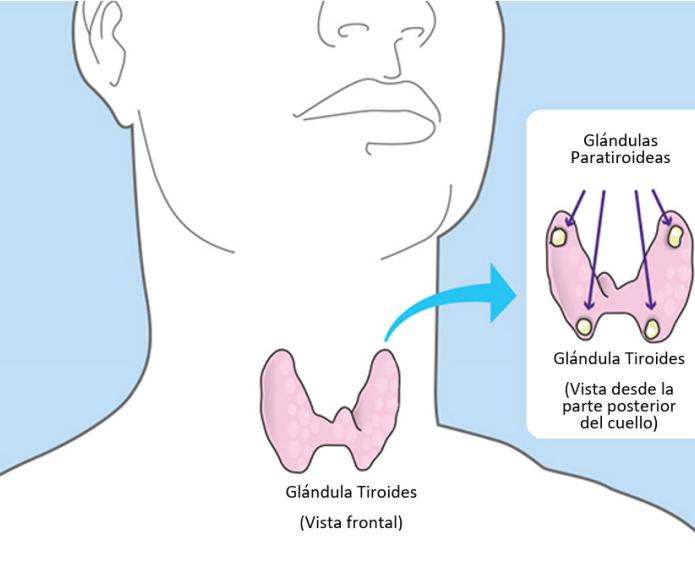
Hyperparathyroidism occurs when the parathyroid glands, which normally regulate calcium balance, produce excessive amounts of hormone, leading to hypercalcemia (elevated levels of calcium in the blood). There are two main types of hyperparathyroidism:
- Primary hyperparathyroidism: Occurs when one or more parathyroid glands become overactive, increasing PTH production without an apparent cause. This form is associated with elevated blood calcium levels and is more common in older adults.
- Secondary hyperparathyroidism: It is a compensatory response to low blood calcium levels and is usually a consequence of other conditions, such as chronic kidney disease or vitamin D deficiency.
Sustained elevation of calcium levels in the body can affect multiple organs, particularly the kidneys, bones, and the cardiovascular system, increasing the risk of serious conditions such as stroke.
Relationship Between Hyperparathyroidism and Stroke
The relationship between hyperparathyroidism and the risk of stroke is primarily related to the effect of elevated calcium levels on blood vessels and blood pressure. The following mechanisms explain this association:
- Arterial hypertension: increased calcium levels in the blood may promote hypertension, as calcium influences vascular smooth muscle contraction, leading to elevated blood pressure and, consequently, an increased risk of stroke.
- Vascular calcification: elevated calcium levels may lead to the accumulation of calcium deposits in the arterial walls, a process known as vascular calcification. This results in arterial stiffening and reduced vascular compliance, increasing the likelihood of thrombus formation and the risk of ischemic stroke.
- Thrombotic risk: imbalance in calcium and other minerals increases the likelihood of blood clot formation. If these clots reach the brain, they can occlude a cerebral vessel and result in a stroke.
- Long-term cardiovascular damage: hyperparathyroidism has also been associated with an increased risk of cardiac arrhythmias and coronary artery disease, conditions that indirectly raise the likelihood of stroke.
Symptoms of hyperparathyroidism
The symptoms of hyperparathyroidism vary depending on disease severity and the duration of elevated calcium levels. Common symptoms include:
- Fatigue and weakness: individuals with hyperparathyroidism often experience excessive fatigue and muscle weakness, which may limit their daily activities.
- Bone pain and fractures: calcium loss from bones weakens bone tissue, increasing the risk of osteoporosis and fractures in individuals with hyperparathyroidism.
- Renal complications: hypercalcemia may lead to the formation of kidney stones and, over time, to renal insufficiency.
- Nausea and loss of appetite: elevated calcium levels affect the gastrointestinal system, leading to stomach discomfort, nausea, and weight loss.
- Neurocognitive changes: confusion, memory impairment, and, in severe cases, depression and anxiety.
- Cardiovascular symptoms: such as hypertension and palpitations, which are closely associated with an increased risk of stroke.
These symptoms are typically progressive, and early detection is important to prevent serious complications, such as stroke.
Diagnosis of hyperparathyroidism
The diagnosis of hyperparathyroidism includes a combination of laboratory tests and imaging studies. The most common assessments include:
- Blood tests: measure serum calcium, phosphorus, and parathyroid hormone (PTH) levels. The diagnosis of hyperparathyroidism is confirmed when elevated calcium levels are observed together with increased PTH levels.
- Vitamin D testing: since low vitamin D levels can induce a compensatory increase in PTH, it is important to measure this vitamin to rule out secondary hyperparathyroidism.
- Parathyroid ultrasound: used to localize enlarged or abnormal glands that may be responsible for increased PTH secretion.
- Bone densitometry: evaluates bone mineral density to determine whether excess PTH is weakening bone tissue.
- Electrocardiogram (ECG): may be performed to assess the impact on the cardiovascular system and determine whether there is any additional risk for the patient.
Treatment and management of hyperparathyroidism to reduce stroke risk
The treatment of hyperparathyroidism depends on the underlying cause, symptom severity, and the risk of complications. Treatment options include:
- Parathyroid surgery: in cases of primary hyperparathyroidism, parathyroidectomy (removal of one or more parathyroid glands) is the most effective option to reduce PTH and calcium levels.
- Calcium-lowering medications: drugs such as bisphosphonates help reduce serum calcium levels and may be useful when surgery is not a viable option.
- Blood pressure control: since hyperparathyroidism increases the risk of hypertension, it is essential to monitor and manage blood pressure to reduce the risk of stroke.
- Dietary and lifestyle modifications: a low-calcium diet and adequate fluid intake help regulate calcium levels. Additionally, reducing sodium intake and engaging in regular physical activity contribute to improved cardiovascular health.
- Vitamin D and phosphorus supplementation: in some cases of secondary hyperparathyroidism, these supplements may be recommended to balance calcium metabolism and reduce PTH production.
These treatments help reduce calcium levels and the risk of vascular calcification, thereby decreasing the likelihood of stroke.
Conclusion
Hyperparathyroidism, particularly when untreated, can have a significant impact on the cardiovascular system and increase the risk of stroke. The relationship between hyperparathyroidism and stroke is primarily mediated by hypercalcemia and its effects on blood pressure, blood vessels, and thrombus formation. Given that the symptoms of hyperparathyroidism can be subtle and progressive, early diagnosis and appropriate treatment are essential to prevent serious complications.
Understanding and management of hyperparathyroidism, along with regular cardiovascular monitoring, are key to reducing the risk of stroke and improving the quality of life of affected individuals.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields