Dysphagia is a disorder that affects the ability to swallow and may occur at any stage of the swallowing process. One of the less recognized, yet equally important forms is esophageal stage dysphagia, a condition that occurs when food has already passed through the mouth and pharynx but encounters difficulty descending through the esophagus to the stomach.
Esophageal stage dysphagia not only causes physical discomfort, but can also compromise nutrition and quality of life.
What is esophageal stage dysphagia?
Swallowing is a complex process that involves several phases: oral preparatory, oral propulsive, pharyngeal, and esophageal. The esophageal stage begins when the food bolus passes from the upper esophageal sphincter into the esophagus and ends when it reaches the stomach. During this stage, the muscles of the esophagus contract in a series of movements known as peristalsis, which propel the food downward.
When these peristaltic movements are impaired or mechanical obstructions are present, what is known as esophageal stage dysphagia occurs. Unlike other forms of dysphagia, the individual may experience the sensation that food is “stuck” in the chest, even after chewing and swallowing properly.
Symptoms of esophageal stage dysphagia
The symptoms of esophageal stage dysphagia are usually quite characteristic, although they are sometimes confused with gastric or respiratory conditions. Among the most common signs are:
-
Sensation of obstruction or pressure in the lower chest
-
Pain during swallowing (odynophagia)
-
Regurgitation of undigested food
-
Persistent hiccups after eating
-
Coughing or throat clearing after meals
-
Unintentional weight loss
-
Difficulty swallowing solids, which may progress to difficulty swallowing liquids
In more advanced cases, there may be episodes of aspiration secondary to reflux, which increases the risk of pneumonia.
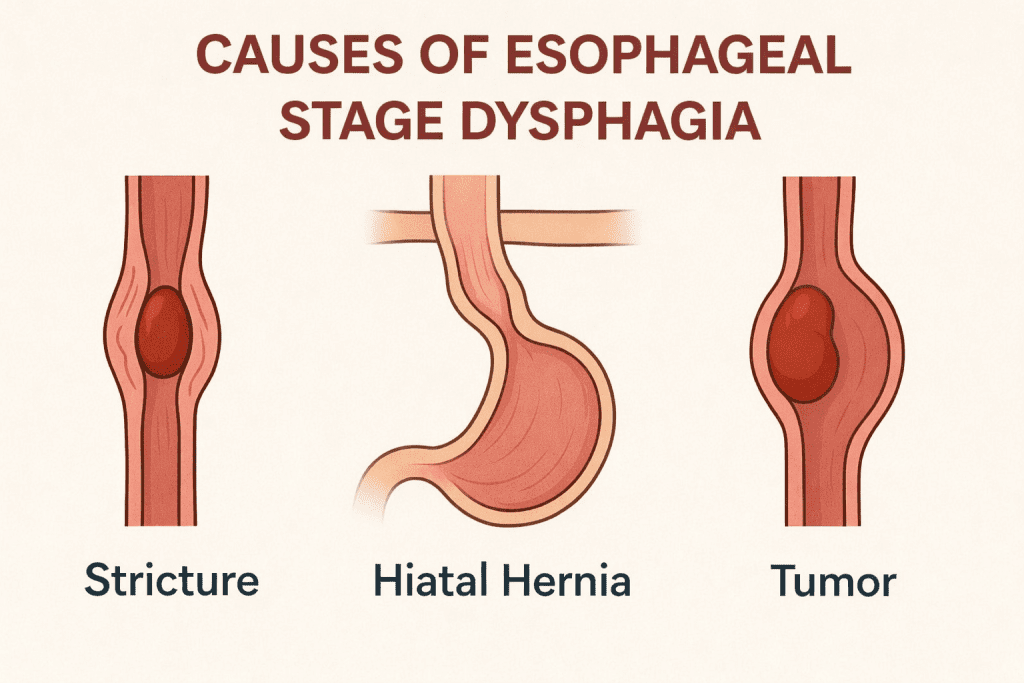
Causes of esophageal stage dysphagia
Esophageal stage dysphagia may be caused by two main types of factors: mechanical (structural) or functional (motility-related).
Mechanical causes:
These involve a partial or complete obstruction of the bolus passage through the esophagus.
-
Esophageal stricture: narrowing of the esophagus due to chronic inflammation or acid reflux.
-
Esophageal rings or webs: abnormal structures that obstruct the passage.
-
Esophageal tumors: benign or malignant
-
Advanced achalasia: dilation of the esophagus that impairs emptying
-
Extrinsic compression: due to aneurysms, mediastinal tumors, or goiter
Functional causes:
They affect esophageal motility, that is, the coordinated movement of its muscles.
-
Achalasia: a disorder of the lower esophageal sphincter, which fails to relax properly.
-
Diffuse esophageal spasm: disorganized and painful contractions
-
Systemic sclerosis: an autoimmune disease that affects the esophageal muscles
-
Esophageal myopathies or neuropathies: secondary to conditions such as diabetes, Parkinson’s disease, ALS, etc.
Diagnosis of esophageal stage dysphagia
The diagnosis of esophageal stage dysphagia requires a specific evaluation, as symptoms do not always manifest in the mouth or throat.
Key diagnostic methods:
-
Upper gastrointestinal endoscopy (UGE)
-
It allows visualization of the interior of the esophagus and detection of strictures, tumors, inflammation, or foreign bodies.
-
-
Barium esophagogram
-
Contrast radiography used to evaluate bolus transit and detect obstructions or motility disorders.
-
-
Esophageal manometry
-
Study of esophageal pressure and muscular coordination, useful for diagnosing achalasia or spasms.
-
-
Esophageal pH monitoring
-
It measures acid reflux and is useful in cases where reflux esophagitis is suspected.
-
-
Clinical and nutritional assessment
-
Medical history, physical examination, assessment of weight loss, etc.
-
A precise diagnosis allows differentiation of esophageal stage dysphagia from other digestive or respiratory disorders and helps guide appropriate treatment.
Treatment of esophageal stage dysphagia
Treatment depends on the underlying cause, the severity of the condition, and the patient’s overall status. Management strategies may be medical, dietary, or surgical.
1. Pharmacological treatment
-
Proton pump inhibitors (PPIs): in cases of reflux esophagitis.
-
Nitrates or calcium channel blockers: for esophageal spasms.
-
Muscle relaxants: in certain motility disorders
2. Endoscopic dilation
-
Indicated for benign strictures. A controlled dilation of the narrowed area is performed using endoscopy.
3. Surgery
-
Heller myotomy: for achalasia
-
Tumor resection or reconstruction: in cases of cancer or severe obstruction
4. Dietary modifications
-
Texture modification (soft or pureed foods)
-
Avoid dry, hard, or sticky foods
-
Eat in an upright position, slowly, and in small amounts
-
Adequate hydration and avoidance of very cold or very hot beverages
5. Enteral nutrition
In severe cases or when there is a risk of aspiration, the use of feeding tubes (nasogastric tube or gastrostomy) may be required.
Rehabilitation and follow-up
The management of esophageal stage dysphagia does not end with the initial treatment. Ongoing clinical follow-up is essential and, in many cases, requires the involvement of a multidisciplinary team:
-
Speech-language pathologists: for swallowing re-education and compensatory strategies
-
Nutritionists: to prevent malnutrition and adapt the diet
-
Gastroenterologists: for endoscopic follow-up and treatment management
-
Psychologists: in cases where the emotional impact of dysphagia is significant
Regular follow-up allows treatment adjustments, helps prevent complications, and supports maintaining a good quality of life.
Complications of untreated esophageal dysphagia
Ignoring or underestimating the symptoms of esophageal stage dysphagia can lead to serious consequences:
-
Weight loss and malnutrition
-
Chronic dehydration
-
Pulmonary aspiration and pneumonia
-
Complete esophageal obstruction
-
Esophageal cancer not diagnosed in time
Therefore, in the presence of any persistent symptoms of difficulty swallowing or a sensation of food “sticking” when eating, it is essential to consult a specialist.
Conclusion
Esophageal stage dysphagia is a complex condition that requires precise evaluation and targeted treatment. Although many people associate dysphagia with throat-related problems, the reality is that a significant proportion of cases originate in the esophagus. Correctly identifying this stage is essential to prevent serious complications and improve the patient’s quality of life.
With a multidisciplinary approach, accurate diagnosis, and personalized treatment, most cases of esophageal stage dysphagia can be effectively managed, allowing for safe and adequate nutrition.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields