Dysphagia is a disorder that affects swallowing, that is, the ability to safely and effectively swallow food, liquids, or even saliva. This condition may result from various neurological, structural, or functional causes, and it has a direct impact on the patient’s health, nutrition, and quality of life. Understanding the stages of dysphagia is essential for both accurate diagnosis and appropriate therapeutic management.
What is dysphagia?
Dysphagia is an impairment in any phase of the swallowing process. It may present as difficulty initiating swallowing, a sensation of food getting stuck, coughing during swallowing, a wet or gurgling voice, or even episodes of pulmonary aspiration. It is important to clarify that dysphagia is not a disease itself, but rather a symptom of various clinical conditions, such as:
-
Stroke (cerebrovascular accident, CVA)
-
Parkinson’s disease
-
Alzheimer’s disease and other dementias
-
Multiple sclerosis or amyotrophic lateral sclerosis (ALS)
-
Head and neck cancer
-
Oropharyngeal surgeries or tracheostomies
-
Degenerative processes or aging
To fully understand this disorder, it is essential to know the stages of dysphagia and how they are classified according to the phase of the swallowing process that is affected.
Stages of swallowing and their relationship with dysphagia
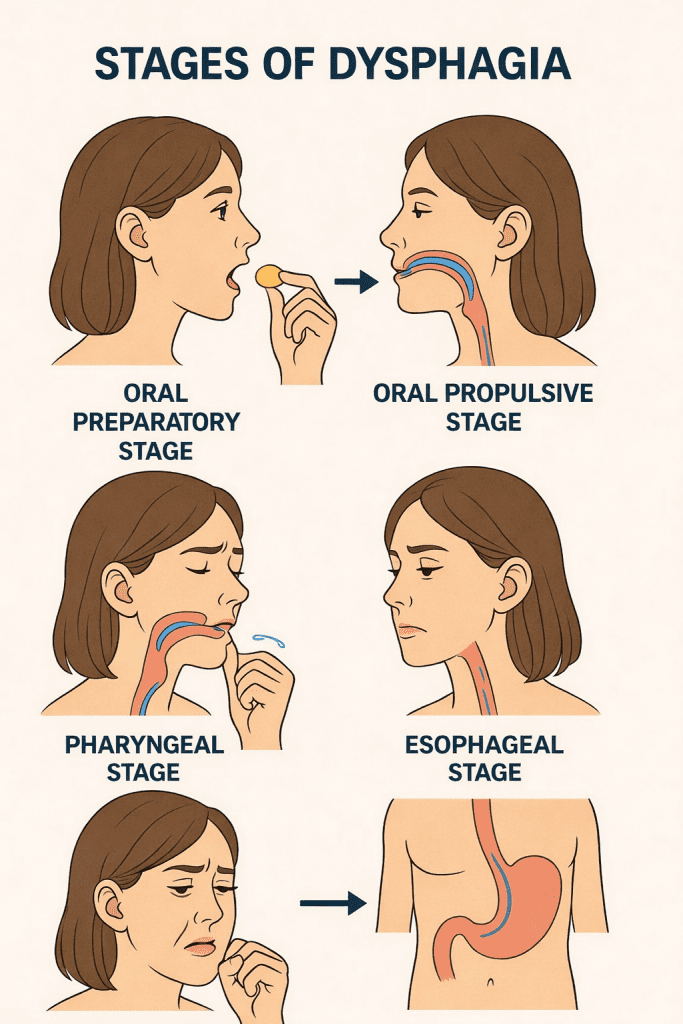
Swallowing is a complex process that is traditionally divided into four stages, each of which may be impaired in dysphagia. Therefore, discussing the stages of dysphagia involves identifying in which phase the alteration occurs:
1. Oral preparatory stage
This is the initial phase of the process, in which food is introduced into the mouth, chewed, and mixed with saliva to form the food bolus. The tongue and the muscles of the jaw, cheeks, and lips play a central role in this stage.
Dysphagia in the oral preparatory stage:
-
Difficulty chewing
-
Food leakage from the lips
-
Food accumulation in the gums or under the tongue
-
Poor bolus formation
Common causes: muscle weakness, tooth loss, facial paralysis, neuromuscular disorders, oral surgery.
Treatment: orofacial exercises, modification of food texture, use of adaptive utensils.
2. Oral propulsive stage (or oral transit)
Once the bolus is formed, the tongue propels it posteriorly toward the pharynx. This stage lasts approximately one second, but it is critical for the efficient passage of food into the esophagus.
Dysphagia in the oral propulsive stage:
-
Inability to initiate swallowing
-
Delayed bolus transit
-
Retention of food in the oral cavity
-
Uncontrolled spillage of the bolus into the pharynx
Common causes: neurological damage (due to stroke, ALS), ankyloglossia, tongue surgery.
Treatment: lingual re-education, postural adjustments, sensory stimulation
3. Pharyngeal stage
This is the most critical phase of the swallowing process, as it involves closure of the airway (larynx) and the passage of the bolus through the pharynx into the esophagus. It relies on highly precise automatic reflexes.
Dysphagia in the pharyngeal stage:
-
Coughing during or after swallowing
-
Voice changes (wet voice)
-
Aspiration of food into the airways
-
Recurrent respiratory infections (pneumonia)
Common causes: brainstem damage, neuromuscular diseases, surgeries involving the neck or pharynx.
Treatment: swallowing maneuvers (such as the supraglottic swallow), pharyngeal reflex exercises, and thickening of liquids
4. Esophageal stage
This is the final stage of the process, in which the bolus travels down the esophagus to the stomach through peristaltic movements.
Dysphagia in the esophageal stage:
-
Sensation of food stuck in the chest
-
Regurgitation
-
Chest pain during swallowing
-
Gastroesophageal reflux
Common causes: achalasia, esophageal stricture, severe reflux, esophageal cancer.
Treatment: medical or surgical intervention, fractionated diet, maintaining an upright position for a prolonged period after eating, proton pump inhibitors
Assessment of the stages of dysphagia
To determine which stages of dysphagia are impaired, different assessment methods are used:
1. Clinical swallowing assessment (CSA)
-
Performed by a speech-language pathologist or swallowing therapist.
-
It includes observation, patient interview, and trials with different types of foods and liquids.
2. Videofluoroscopic swallowing study (VFSS)
-
Dynamic radiographic study of the swallowing process using contrast.
-
It allows precise identification of the phase in which the disorder occurs.
3. Fiberoptic nasopharyngolaryngoscopy
-
A minimally invasive technique that allows direct visualization of the larynx and pharynx during swallowing.
4. Esophageal manometry
-
It assesses pressure and motility in the esophagus and is useful for confirming esophageal dysphagia.
Treatment according to the stages of dysphagia
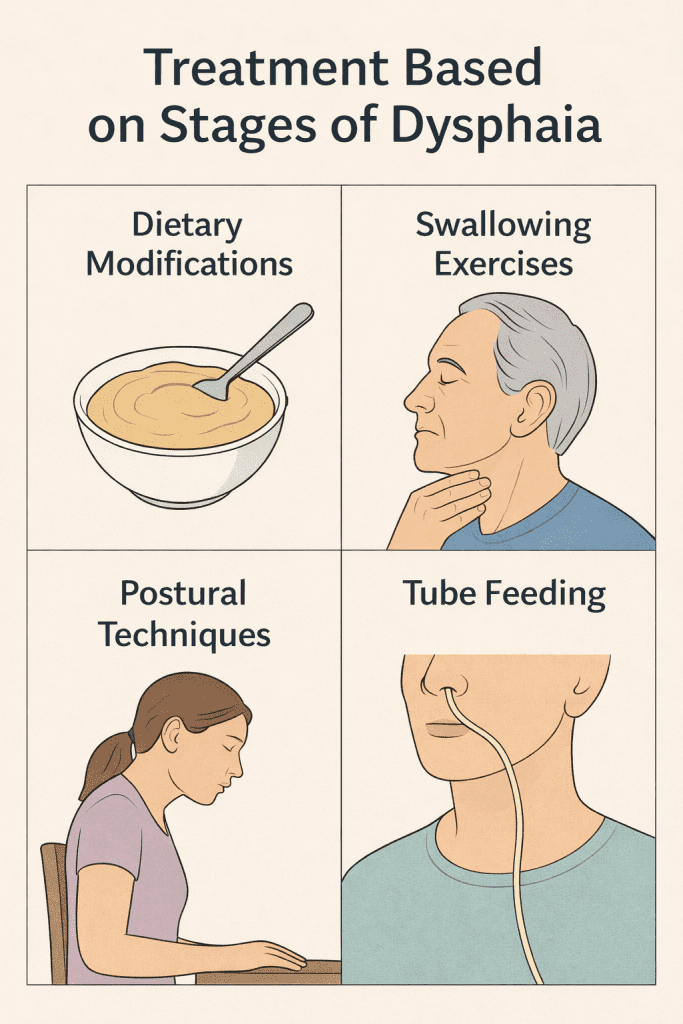
The treatment of dysphagia must be individualized and tailored to the affected stages. A multidisciplinary approach is essential: speech-language pathologists, nutritionists, neurologists, otolaryngologists, and gastroenterologists should work together.
Common interventions:
-
Texture modification (thickened liquids, pureed foods, mechanically soft diet).
-
Myofunctional exercises for the tongue, lips, and jaw.
-
Swallowing reflex retraining
-
Postural management and compensatory techniques (head tilt, double swallowing, etc.).
-
Thermal and tactile stimulation
-
Enteral nutrition (nasogastric tube or gastrostomy) in severe cases of dysphagia
Complications of not properly managing the stages of dysphagia
Ignoring the signs of dysphagia or intervening without correctly identifying the affected stage can lead to serious consequences:
-
Aspiration pneumonia
-
Malnutrition and weight loss
-
Dehydration
-
Food aversion and anxiety during eating
-
Social isolation
-
Increased morbidity in elderly or neurologically impaired patients
Therefore, identifying the stages of dysphagia is not just a clinical exercise, but a fundamental step in preserving the patient’s health and life.
Conclusion
Conocer y diferenciar las etapas de la disfagia permite un enfoque diagnóstico y terapéutico mucho más preciso. Cada fase de la deglución implica funciones distintas y requiere intervenciones específicas cuando se ve comprometida.
El abordaje debe ser temprano, multidisciplinar y continuo. Con una correcta evaluación y tratamiento adaptado, muchas personas con disfagia pueden recuperar una alimentación segura y mejorar notablemente su calidad de vida. En definitiva, entender las etapas de la disfagia es el primer paso hacia una rehabilitación efectiva y una vida digna para quienes enfrentan este desafío.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields