Swallowing is a complex and highly coordinated process that enables the safe transit of food and liquids from the oral cavity to the stomach. This process consists of several stages, one of the most critical being the pharyngeal phase. When this stage is impaired, pharyngeal stage dysphagia occurs, a disorder that can compromise swallowing safety and increase the risk of pulmonary aspiration, respiratory infections, or malnutrition.
Understanding pharyngeal stage dysphagia is essential to achieve early diagnosis, implement effective treatments, and prevent serious complications.
What is pharyngeal stage dysphagia?
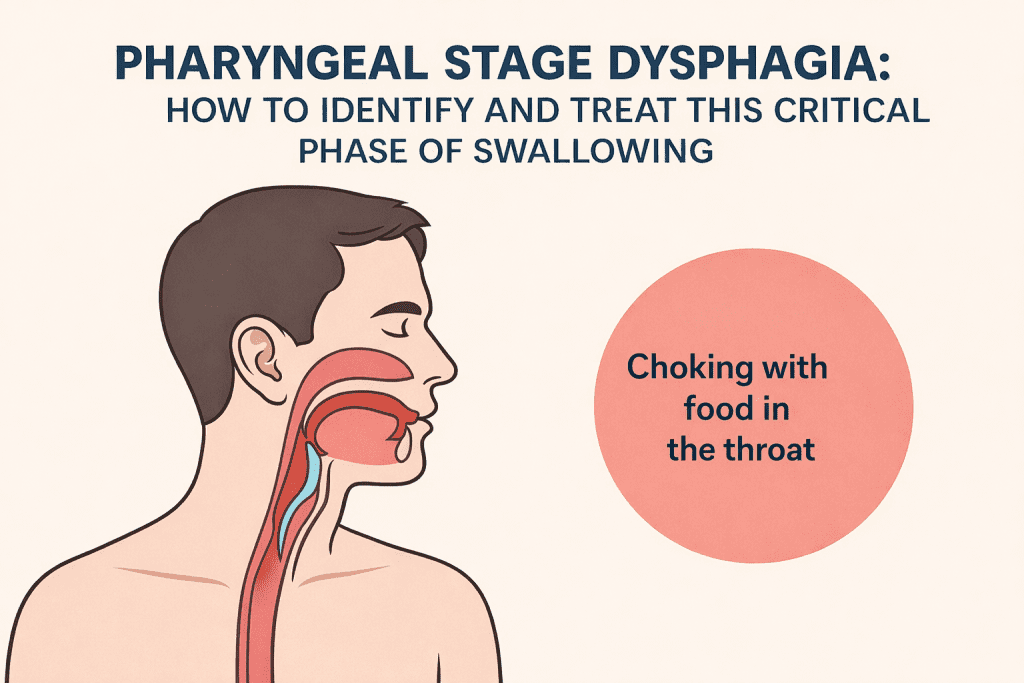
Pharyngeal stage dysphagia is an impairment in the pharyngeal phase of swallowing, which begins when the food bolus reaches the posterior oral cavity and triggers the swallowing reflex, passing through the pharynx toward the esophagus. This phase lasts only about one second, but requires precise coordination of multiple muscles and automatic reflexes, such as airway closure and laryngeal elevation.
When this coordination is impaired, pharyngeal stage dysphagia develops, with the risk that food or liquid enters the airway instead of the esophagus.
Symptoms of pharyngeal stage dysphagia
Clinical signs of pharyngeal stage dysphagia may vary depending on the severity of the disorder, but some of the most common include:
-
Coughing during or immediately after swallowing
-
Sensation of choking or gagging
-
Voice changes after eating (wet or gurgly voice)
-
Fragmented swallowing or swallowing with prolonged pauses
-
Sensation of food sticking in the throat
-
Nasal regurgitation during liquid swallowing
-
Fever of unknown origin associated with microaspiration
-
Recurrent respiratory infections, such as aspiration pneumonia
-
Weight loss and reduced oral intake
In severe cases, pharyngeal dysphagia may lead the individual to avoid eating due to fear of choking.
Causes of pharyngeal stage dysphagia
Pharyngeal stage dysphagia typically has a neurological or structural origin. The most common causes include:
1. Stroke
-
Brainstem or cerebral hemisphere lesions that interfere with the neural control centers of swallowing
2. Neurodegenerative diseases
-
Parkinson’s disease, Alzheimer’s disease, amyotrophic lateral sclerosis (ALS), and multiple sclerosis can lead to impaired coordination of pharyngeal reflexes
3. Traumatic brain injury
-
Injuries at the skull base or in motor speech areas may affect the pharyngeal phase
4. Head and neck surgeries or tumors
-
Surgical interventions in the pharynx or radiotherapy may damage structures and nerves involved in swallowing
5. Myopathies or myasthenia gravis
-
Muscle disorders that weaken the muscles involved in the swallowing reflex
6. Congenital disorders
-
Cerebral palsy or neuromotor syndromes in children
Diagnosis of pharyngeal stage dysphagia
Accurate diagnosis is essential to identify the type of dysphagia and guide treatment. The most commonly used tools to detect pharyngeal stage dysphagia include:
1. Clinical swallowing assessment (CSA)
-
Initial evaluation performed by a speech and language therapist, observing the patient’s swallowing behavior with different food consistencies
2. Videofluoroscopic swallowing study (VFSS)
-
Radiological technique that allows real-time visualization of the bolus transit from the oral cavity to the esophagus. It is the most sensitive method for detecting aspiration and delays in the pharyngeal reflex.
3. Fiberoptic endoscopic evaluation of swallowing (FEES)
-
Insertion of a flexible endoscope through the nasal passage to visualize the pharynx and larynx during swallowing. It is ideal for identifying residue and laryngeal penetration.
4. Pharyngoesophageal manometry
-
Measures muscle pressure during swallowing and evaluates the coordination of the upper sphincters
Treatment of pharyngeal stage dysphagia
The management of pharyngeal stage dysphagia depends on the underlying cause, severity, and patient functional status. It requires a multidisciplinary approach involving speech and language therapists, rehabilitation physicians, neurologists, nutritionists, and nursing staff.
1. Swallowing therapy
-
Pharyngeal exercises to strengthen the muscles involved
-
Thermal and tactile stimulation to facilitate the swallowing reflex
-
Compensatory swallowing maneuvers, such as:
-
Supraglottic maneuver: protects the airway
-
Mendelsohn maneuver: improves laryngeal elevation
-
Effortful swallow or double swallow
-
2. Postural modifications
-
Head flexion (chin tuck) to reduce the risk of aspiration
-
Head rotation toward the affected side to facilitate bolus transit
3. Dietary modifications
-
Texture-modified diets: pureed foods, homogeneous consistencies, and thickened liquids
-
Elimination of foods that are crumbly or sticky
4. Enteral nutrition
-
In severe cases, feeding via nasogastric tube or temporary gastrostomy may be indicated
5. Adjunctive therapies
-
Neuromuscular electrical stimulation (NMES) (VitalStim)
-
Biofeedback with visualization of the swallowing reflex
Rehabilitation and prognosis
Pharyngeal stage dysphagia may improve with appropriate treatment, although prognosis depends on multiple factors:
-
Patient age
-
Etiology (neurological, structural, muscular)
-
Duration of the condition
-
Cognitive status
-
Access to a specialized rehabilitation team
In many cases, patients achieve partial or complete recovery of safe swallowing function. Rehabilitation should be initiated as early as possible to prevent complications such as aspiration pneumonia or malnutrition.
Complications of untreated pharyngeal dysphagia
Failure to adequately manage pharyngeal stage dysphagia may lead to serious complications:
-
Aspiration pneumonia: the leading cause of death in untreated dysphagia
-
Malnutrition and loss of muscle mass
-
Dehydration
-
Feeding dependency
-
Social isolation and depression
The impact extends beyond the physical: many individuals withdraw from social or family events due to fear of choking.
Conclusion
Pharyngeal stage dysphagia is a potentially dangerous condition that affects the most critical phase of swallowing. Early identification and a comprehensive therapeutic approach can make the difference between a life with constant aspiration risk and a satisfactory functional recovery.
A multidisciplinary team, individualized therapies, and family support are key pillars for recovery. Early detection of signs and prompt intervention can prevent serious complications and significantly improve the patient’s quality of life.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields