Histotoxic hypoxia is a specific type of hypoxia that occurs when body cells are unable to utilize the available oxygen, despite adequate oxygen levels in the blood. This form of hypoxia is less well known than hypoxic or ischemic hypoxia, but it can have equally devastating consequences for health, especially if not identified and treated in a timely manner.
What is histotoxic hypoxia?
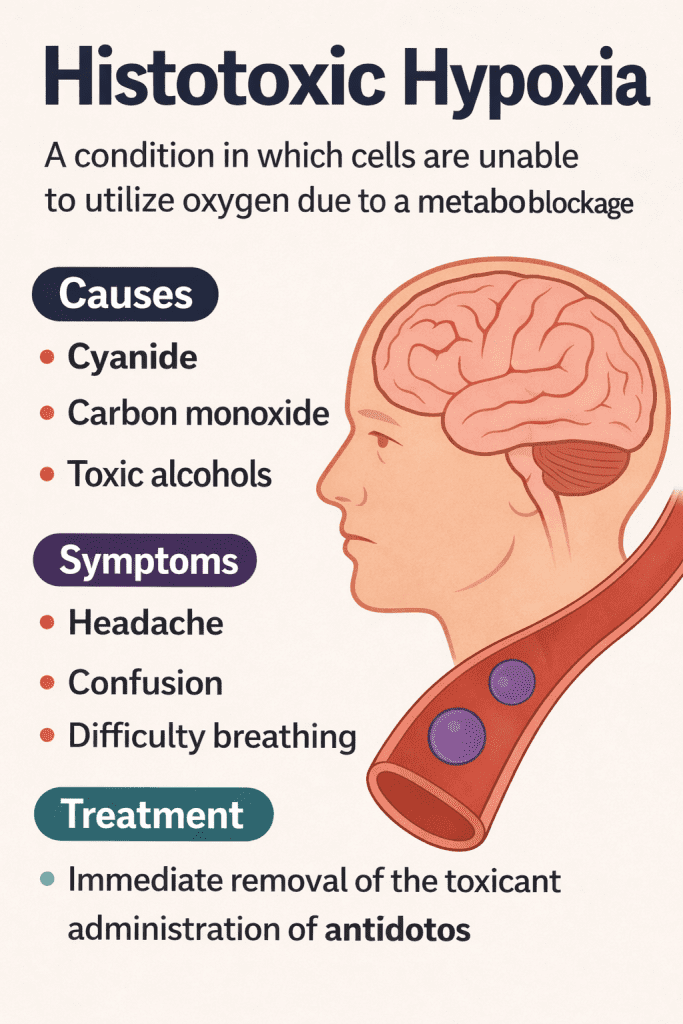
The term histotoxic hypoxia derives from the Greek word histos (tissue) and the suffix -toxic (harmful or poisonous). It refers to a condition in which oxygen is present in normal amounts in the bloodstream, but cells are unable to utilize it because the process of cellular respiration is impaired. In other words, it is not a lack of oxygen in the environment, but a metabolic inability to properly process it.
Histotoxic hypoxia primarily affects the mitochondria, the cellular organelles responsible for converting oxygen and nutrients into energy (ATP). If the mitochondria are inhibited by a toxic substance, as occurs in certain types of poisoning, energy production is halted, which can lead to progressive cellular and organ failure.
Main causes of histotoxic hypoxia
Histotoxic hypoxia is caused almost exclusively by toxic agents that interfere with cellular oxygen metabolism. Among the most well known are:
-
Cyanide: It is the classic toxin associated with histotoxic hypoxia. Cyanide inhibits the enzyme cytochrome c oxidase in the mitochondrial electron transport chain, thereby blocking ATP production.
-
Carbon monoxide (CO): Although it is often associated with anemic hypoxia, it can also produce effects similar to histotoxic hypoxia by binding to mitochondrial enzymes and impairing oxygen utilization.
-
Toxic alcohols: Methanol and ethylene glycol can generate metabolites that impair cellular metabolism, contributing to a mixed clinical picture that includes features of histotoxic hypoxia.
-
Certain medications and drugs: Substances such as amobarbital or certain pesticides may, in rare cases, interfere with cellular respiration.
-
Genetic defects or mitochondrial diseases: Although much less common, they can also trigger processes similar to histotoxic hypoxia by affecting the enzymes required for oxygen metabolism.
Pathophysiological mechanism of histotoxic hypoxia
Under normal conditions, oxygen is delivered to the tissues, enters the cells, and reaches the mitochondria, where it is essential for oxidative phosphorylation. In histotoxic hypoxia, although oxygen is present in arterial blood and reaches the tissues, the mitochondria are unable to utilize it due to biochemical interference, such as that caused by cyanide.
This leads to a collapse in ATP production, forcing cells to rely on anaerobic glycolysis for energy. As a result, lactic acid accumulates, leading to severe metabolic acidosis. If the underlying cause of histotoxic hypoxia is not rapidly reversed, cells die due to energy failure.
Symptoms of histotoxic hypoxia
Symptoms may vary depending on the causative agent and the rate of exposure, but generally include:
-
Severe headache
-
Nausea and vomiting
-
Mental confusion or disorientation
-
Shortness of breath despite normal blood oxygen levels
-
Tachycardia
-
Loss of consciousness
-
Seizures
-
In severe cases, coma and death
A distinctive feature of histotoxic hypoxia is that the blood may appear bright red, as oxygen has not been utilized by the tissues and returns through the veins without significant change.
Diagnosis of histotoxic hypoxia
The diagnosis of histotoxic hypoxia is primarily clinical and by exclusion. It is typically suspected in patients exposed to toxic substances who present signs of hypoxia despite normal arterial oxygenation. Diagnostic evaluation includes:
-
Arterial blood gas analysis: may show metabolic acidosis and elevated lactate levels.
-
Elevated central venous oxygen saturation: indicating that oxygen has not been adequately extracted by the tissues.
-
Toxicological analysis: to detect the presence of cyanide, carbon monoxide, or other substances.
-
Neurological assessment: to evaluate the impact of brain injury due to prolonged hypoxia.
Treatment of histotoxic hypoxia
The treatment of histotoxic hypoxia depends on the underlying cause. The most common strategies include:
-
Immediate removal of the toxin: the first step is to stop exposure by transferring the patient to a safe and well-ventilated environment.
-
Oxygen therapy: although it does not resolve the underlying problem on its own, high concentrations of oxygen (including hyperbaric oxygen) may help counteract the toxin and improve cellular metabolism.
-
Specific antidotes:
-
In cases of cyanide poisoning, hydroxocobalamin, sodium thiosulfate, or sodium nitrite may be administered.
-
For carbon monoxide poisoning, hyperbaric oxygen therapy is the treatment of choice.
-
-
Advanced life support: includes airway management, fluid therapy, seizure control, and treatment of acidosis.
-
Hemodialysis: in cases of poisoning with toxic alcohols or other dialyzable compounds.
Prognosis and sequelae
The prognosis of histotoxic hypoxia depends on the speed of diagnosis and treatment. Early intervention can prevent permanent damage. However, if exposure is prolonged or the patient does not receive appropriate care, severe sequelae may develop, such as:
-
Irreversible neurological damage
-
Cognitive impairments
-
Movement disorders
-
Multiorgan failure
The central nervous system is particularly vulnerable, making neurological follow-up essential.
Prevention of histotoxic hypoxia
Histotoxic hypoxia can be primarily prevented by avoiding exposure to toxic substances. Some recommendations include:
-
Store and handle chemical products safely.
-
Use appropriate protective equipment in industrial or agricultural environments.
-
Avoid the use of gas heaters in enclosed spaces.
-
Carbon monoxide detectors in the home.
-
Medical supervision when using medications that may affect mitochondrial metabolism.
-
Education on the risks of cyanide and similar substances in occupational settings.
Conclusion
Histotoxic hypoxia represents a medical emergency that, although less common than other forms of hypoxia, can have equally severe consequences. Recognizing its causes, understanding its mechanisms, and acting rapidly are essential to prevent permanent sequelae. Prevention, education, and the appropriate use of antidotes can make the difference between life and death in the most severe cases. Clinical vigilance, medical expertise, and awareness of toxic risks remain our most effective tools against this silent threat.
Si necesita información sobre NeuroAiD II, puede rellenar este formulario de contacto
"*" indicates required fields