Mechanical thrombectomy in stroke represents one of the most significant advances in modern medicine for the management of ischemic stroke. Since its introduction, it has transformed the prognosis of thousands of patients who would otherwise have been left with severe neurological sequelae. This endovascular procedure offers the possibility of rapidly and effectively restoring cerebral blood flow, significantly reducing long-term disability.
What is mechanical thrombectomy in stroke
Mechanical thrombectomy in stroke is a treatment that involves the direct removal of a blood clot occluding a cerebral artery. Specialized devices such as stent retrievers or aspiration systems are used, which are introduced through a catheter via a peripheral artery, typically the femoral or radial artery. This procedure is primarily indicated in cases of large vessel occlusion, such as the middle cerebral artery or the internal carotid artery, which are associated with large cerebral infarctions.
Indications and selection criteria
Not all patients with ischemic stroke are candidates for mechanical thrombectomy in stroke. Patient selection depends on both clinical and radiological criteria. The main criteria include:
-
Patients with severe neurological symptoms
-
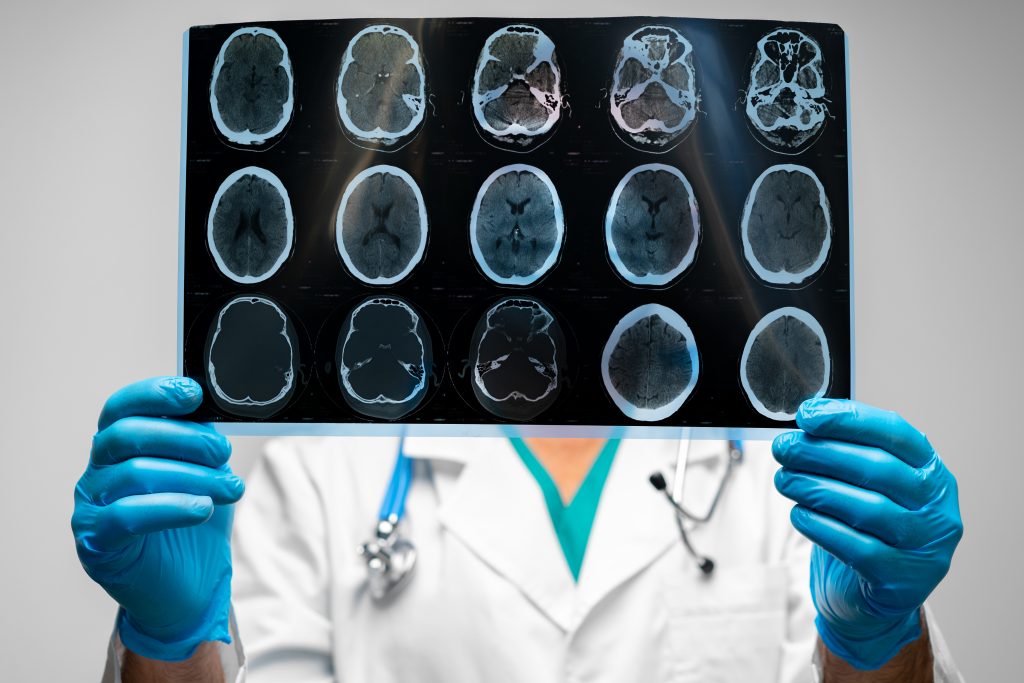
Evidence of large vessel occlusion on neuroimaging (CT or MRI)
-
Symptom onset typically within less than 6 hours, although some studies have extended the therapeutic window up to 16–24 hours in selected cases
-
Absence of extensive established brain damage on neuroimaging
Thanks to these criteria, specialists can identify those patients who are most likely to benefit from the procedure.
How mechanical thrombectomy in stroke is performed
Mechanical thrombectomy in stroke is performed in a catheterization laboratory or an interventional neuroradiology suite. The procedure is carried out under general anesthesia or conscious sedation, depending on the patient’s clinical condition. Through a catheter, the physician advances the devices until reaching the thrombus occluding the cerebral artery. Once located, mechanical extraction is performed, either by capturing the clot with a stent retriever or through direct aspiration. After removal, recanalization is confirmed by cerebral angiography.
Clinical benefits of mechanical thrombectomy in stroke
Mechanical thrombectomy in stroke has demonstrated, in multiple clinical trials and real-world practice, clear benefits compared to treatment with intravenous thrombolysis alone. The most important include:
-
Increased rate of complete recanalization of occluded arteries
-
Significant reduction in disability at 90 days
-
Higher likelihood of functional independence
-
Possibility of treatment even in patients beyond the 4.5-hour window for intravenous thrombolysis
This makes the procedure an essential pillar within ischemic stroke management strategies.
Potential risks and complications
Like any intervention, mechanical thrombectomy in stroke is not without risks. The most common complications include:
-
Secondary intracranial hemorrhage
-
Vascular injury during catheter manipulation
-
Reocclusion of the treated vessel
-
Infections or complications related to vascular access
However, the benefits clearly outweigh the risks when the procedure is performed in appropriately selected patients and in specialized centers.
Mechanical thrombectomy in stroke and subsequent rehabilitation
The success of mechanical thrombectomy in stroke does not end with vessel recanalization. Patient recovery also depends on appropriate rehabilitation. Programs including physiotherapy, occupational therapy, speech therapy, and cognitive neurorehabilitation are essential to maximize functional independence. In addition, early rehabilitation promotes neuroplasticity and reduces long-term sequelae.
Impact on quality of life and public health
The implementation of mechanical thrombectomy in stroke has had a significant impact on public health. It has been shown to reduce disability-adjusted life years, benefiting not only patients and their families, but also healthcare systems by lowering long-term care costs and dependency. In countries where the technique has been systematically implemented, a reduction in mortality and an increase in patients’ return to work have been observed.
Future perspectives of mechanical thrombectomy in stroke
The field of mechanical thrombectomy in stroke continues to evolve. Increasingly effective devices, safer endovascular navigation techniques, and care protocols aimed at reducing door-to-recanalization times are being developed. In addition, research is exploring the combination of this treatment with neuroprotective agents and regenerative therapies to enhance brain recovery. The future points toward faster, more effective, and more accessible procedures across a broader network of hospitals.
Conclusion
Mechanical thrombectomy in stroke has revolutionized the treatment of ischemic stroke by providing an effective tool to restore cerebral blood flow in cases of large vessel occlusion. Its appropriate application, based on clinical and radiological criteria, allows saving lives and drastically reducing neurological sequelae. Although it requires specialized centers and trained teams, its implementation is marking a turning point in the fight against one of the leading causes of disability worldwide.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields