Tissue oxygenation is an essential process for life. Any alteration in the uptake, transport, or utilization of oxygen can compromise cellular function. Among the different forms of hypoxia, anemic hypoxia holds a particular place due to its origin in a common disorder: anemia. This condition affects the blood’s capacity to transport oxygen, even when the lungs and circulatory system are functioning properly.
What is anemic hypoxia?

Anemic hypoxia is a type of hypoxia that occurs when the amount of functional hemoglobin in the blood is insufficient to transport the oxygen required by the tissues. Even if oxygen is available in the air and the lungs are functioning properly, the blood cannot efficiently deliver it due to a deficiency in hemoglobin or a reduced number of red blood cells.
This form of hypoxia is characterized by apparently normal oxygen saturation, but inadequate oxygen delivery at the tissue level. In other words, pulse oximeters may show normal values, while the body is actually experiencing functional oxygen deficiency.
Causes of anemic hypoxia
Anemic hypoxia can be caused by any condition that reduces the oxygen-carrying capacity of the blood. The most common causes include:
-
Iron deficiency anemia: the most common type, caused by iron deficiency.
-
Megaloblastic anemia: caused by deficiencies in vitamin B12 or folic acid.
-
Hemolytic anemia: accelerated destruction of red blood cells.
-
Acute or chronic hemorrhage: significant blood loss.
-
Chronic diseases: renal failure, persistent infections, cancer.
-
Exposure to toxic substances:
-
Carbon monoxide: binds to hemoglobin forming carboxyhemoglobin, which is unable to carry oxygen.
-
Nitrites and nitrates: oxidize hemoglobin to methemoglobin, which is unable to transport oxygen.
-
-
Hereditary disorders: such as thalassemia or sickle cell anemia.
In all these cases, the result is the same: an inadequate amount of functional hemoglobin available to deliver oxygen to the tissues, leading to anemic hypoxia.
Symptoms of anemic hypoxia
The symptoms of anemic hypoxia may vary in intensity depending on the rate of onset and the level of hemoglobin. When hypoxia develops gradually, the body can partially adapt, but in acute cases, symptoms are more pronounced.
General symptoms:
-
Pallor of the skin and mucous membranes
-
Severe fatigue
-
Dyspnea (shortness of breath, even at rest)
-
Palpitations
-
Dizziness or vertigo
-
Headache
-
Cold hands and feet
-
Exercise intolerance
-
Tinnitus (ringing in the ears)
-
Irritability and difficulty concentrating
Neurological or cardiovascular symptoms may occur if anemic hypoxia is severe and prolonged.
Differences between anemic hypoxia and other forms of hypoxia
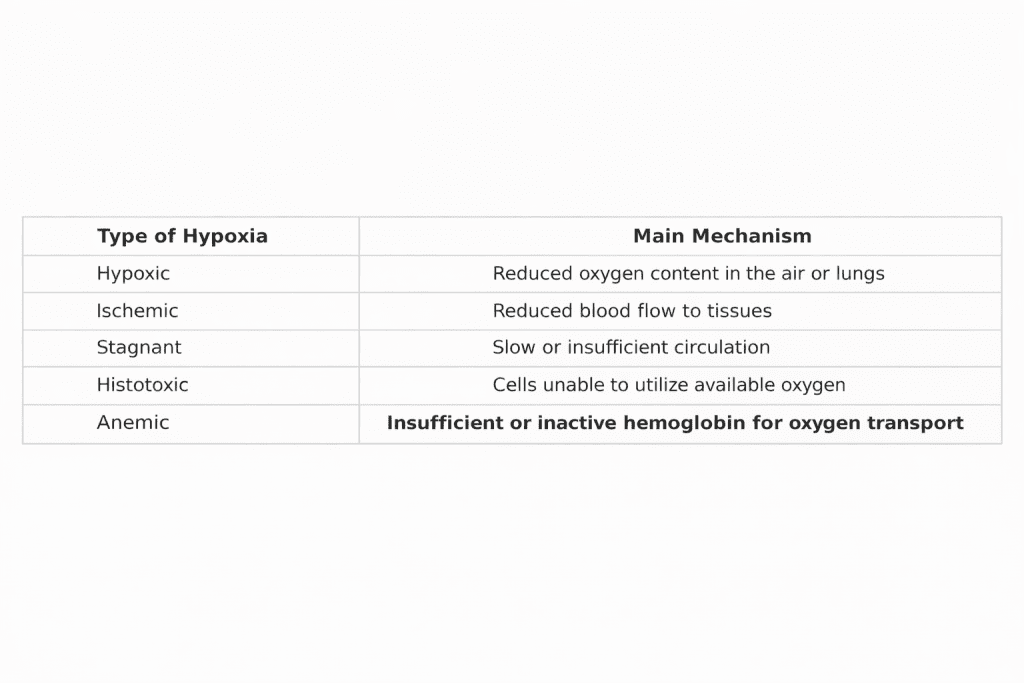

Understanding this difference is key to establishing appropriate treatment.
Diagnosis
The diagnosis of anemic hypoxia includes:
-
Complete blood count (CBC):
-
Decreased hemoglobin, hematocrit, and red blood cell count.
-
Assessment of mean corpuscular volume (MCV), a useful index for classifying the type of anemia.
-
-
Blood gas analysis:
-
Oxygen saturation may be normal.
-
Reduced total arterial oxygen content (CaO₂).
-
-
Ferritin, serum iron, and transferrin:
-
To assess iron deficiency.
-
-
Vitamin B12 and folic acid levels:
-
In suspected megaloblastic anemia.
-
-
Specific tests:
-
Hemoglobin electrophoresis to detect thalassemia or sickle cell disease.
-
Perfecto, pásame el texto cuando quieras.
-
Early diagnosis allows the prevention of major complications such as heart failure or brain damage due to prolonged hypoxia.
Treatment of anemic hypoxia
The treatment of anemic hypoxia is based on addressing the underlying cause and restoring the oxygen-carrying capacity. The options include:
-
Oral or intravenous supplementation:
-
Iron, vitamin B12, folic acid, depending on the type of deficiency.
-
-
Blood transfusions:
-
In cases of acute anemia, hemorrhage, or dangerously low hemoglobin levels.
-
-
Oxygen therapy:
-
Useful as supportive therapy, although limited if hemoglobin is not available.
-
-
Treatment of underlying diseases:
-
Management of renal, autoimmune, or neoplastic diseases.
-
-
Specific antidotes:
-
Methylene blue in cases of methemoglobinemia.
-
Hyperbaric oxygen therapy in cases of carbon monoxide poisoning.
-
-
Lifestyle:
-
Iron- and vitamin-rich diet, cessation of alcohol and tobacco use, treatment of intestinal parasites in endemic areas.
-
Prognosis
The prognosis of anemic hypoxia depends on the underlying cause and the timeliness of treatment. In most cases, it is reversible if the anemia is corrected in time. However, in patients with chronic diseases or continuous exposure to toxins, the risk of permanent damage increases.
In vulnerable populations such as elderly individuals, pregnant women, and patients with cardiovascular diseases, anemic hypoxia can destabilize the organism and increase the risk of mortality.
Prevention
The prevention of anemic hypoxia involves:
-
Early diagnosis of anemia during routine check-ups
-
Preventive supplementation in pregnant women
-
Pediatric nutritional monitoring
-
Prevention and treatment of intestinal parasites
-
Avoid exposure to toxic gases
-
Health education in at-risk populations
A healthcare system with access to basic laboratory testing can rapidly identify anemia and prevent its progression to anemic hypoxia.
Conclusion
Anemic hypoxia is a condition in which body tissues do not receive sufficient oxygen due to a reduction in the quantity or quality of hemoglobin. Although it is a less evident form of hypoxia compared to others, it can have serious consequences if not treated in time.
Recognizing its causes, symptoms, and diagnostic methods allows for effective intervention. Medical education, nutritional prevention, and access to treatment are key to combating this silent yet common form of hypoxia.
Si necesita información sobre NeuroAiD II, puede rellenar este formulario de contacto
"*" indicates required fields