
Swallowing is an essential function for nutrition and hydration, carried out through a sequential process divided into several phases. One of these stages, often overlooked but of high clinical relevance, is the propulsive oral stage. This phase plays a decisive role in the safe and efficient transfer of the food bolus from the oral cavity to the pharynx. When this phase is impaired, it is referred to as propulsive oral stage dysphagia, a condition that can significantly compromise feeding and the patient’s quality of life.
What is the propulsive oral stage?
The propulsive oral stage is the second subphase of the oral stage of swallowing. It occurs immediately after the preparatory phase, in which the food has been chewed and formed into a bolus ready to be swallowed. In this phase, the tongue is responsible for propelling the bolus toward the pharynx through a wave-like motion, while the soft palate seals to prevent reflux into the nasal cavity.
This movement must be rapid, efficient, and well-coordinated. When there is dysfunction in any of the components involved, propulsive oral stage dysphagia occurs, a specific impairment in the transport of the bolus from the oral cavity to the pharynx.
Clinical characteristics of propulsive oral stage dysphagia
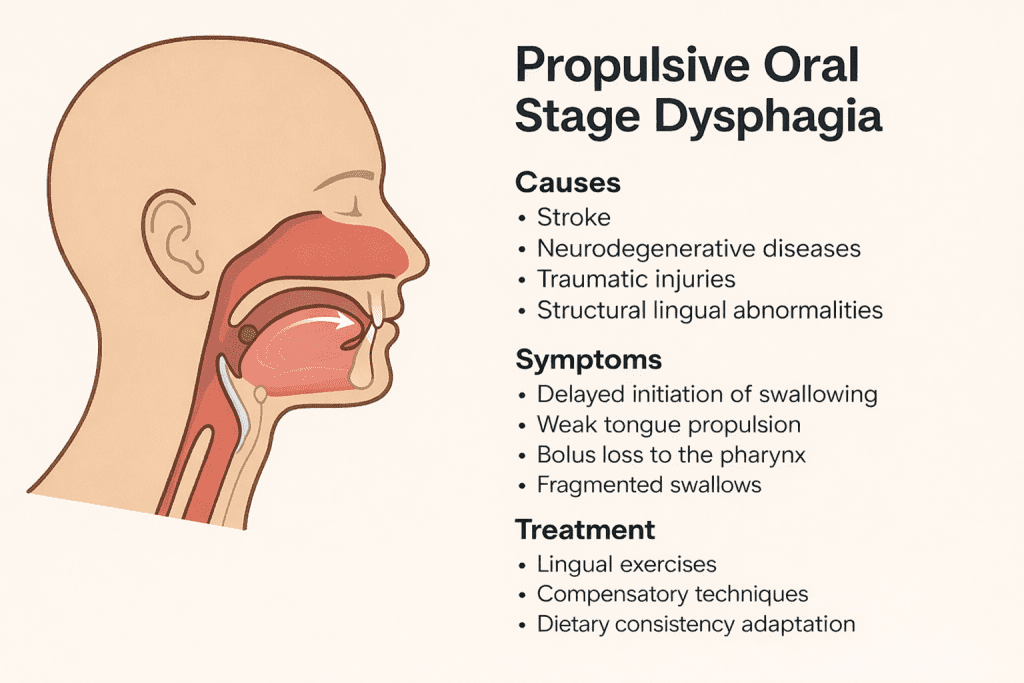
Propulsive oral stage dysphagia presents a set of symptoms that may be confused with impairments in other phases of swallowing. It is crucial to identify this stage as the origin of the problem, as its therapeutic approach is specific. Among the most common symptoms are:
-
Delayed initiation of swallowing.
-
Premature spillage of the bolus into the pharynx before the swallowing reflex.
-
Weak or ineffective lingual propulsion.
-
Increased number of swallows per bolus.
-
Sensation of food remaining trapped in the oral cavity or at the posterior aspect of the tongue.
-
Fractionated swallows.
These symptoms are often exacerbated with mixed-consistency or liquid foods, as they require greater lingual control to prevent premature spillage into the pharynx and risk of aspiration.
Causes of propulsive oral stage dysphagia
The causes of propulsive oral stage dysphagia may be multiple, but in most cases they are related to neuromuscular or structural disorders that affect lingual function and oral motor control. The most common causes are listed below:
-
Stroke: One of the most common factors, especially when the infarction affects cortical areas responsible for lingual control.
-
Neurodegenerative diseases: Parkinson’s disease, amyotrophic lateral sclerosis (ALS), or multiple sclerosis can lead to progressive tongue weakness and loss of fine motor control.
-
Traumatic brain injuries: They may affect brain regions responsible for the planning and motor execution of the tongue.
-
Structural lingual alterations: Such as partial or total glossectomy due to cancer, macroglossia, or severe ankyloglossia.
-
Aging: Age-related lingual sarcopenia can reduce bolus propulsion strength and the coordination required for efficient swallowing.
-
Neuromotor developmental disorders: In the pediatric population, developmental delay or cerebral palsy can cause propulsive oral stage dysphagia from early ages.
Diagnosis of propulsive oral stage dysphagia
The clinical evaluation of this specific form of dysphagia is primarily performed through direct observation and the use of complementary tools. The objective is to assess the effectiveness of lingual movement and its ability to propel the food bolus. Diagnostic methods include:
-
Clinical swallowing evaluation (CSE): Allows observation of lingual control, direction of movement, and the presence of residue in the oral cavity after swallowing.
-
Videofluoroscopic swallowing study (VFSS): A key technique to accurately analyze bolus transit during the oral stage and detect delays or premature spillage before the pharyngeal reflex.
-
Electromyographic evaluation: It may be used in specialized studies to measure the strength and coordination of lingual musculature.
Clinical consequences
Propulsive oral stage dysphagia may appear less dangerous than other forms of dysphagia, but its effects are cumulative and potentially serious if not addressed in a timely manner. Among the most common consequences are:
-
Early aspiration: When the bolus reaches the pharynx without an active swallowing reflex, silent aspiration into the airway may occur.
-
Malnutrition and dehydration: The effort and time required for swallowing may lead to reduced caloric and fluid intake.
-
Fatigue and frustration during eating: Mealtime duration increases and a sense of dependency develops.
-
Risk of respiratory infections: Repeated presence of oral residue and potential aspiration may predispose to aspiration pneumonia.
Therapeutic management of propulsive oral stage dysphagia
The treatment of this disorder is based on neuromuscular rehabilitation, functional compensation, and dietary adaptation. The following strategies can be integrated into a personalized therapeutic plan:
-
Specific lingual exercises: Movements aimed at improving tongue strength and mobility, such as pressing the tongue against a tongue depressor or performing resisted protrusion exercises.
-
Oral massage and stimulation: Thermal and tactile stimulation techniques that help increase oropharyngeal awareness.
-
Compensatory techniques: Postural adjustments, such as anterior head tilt, or techniques such as the effortful swallow maneuver to improve propulsion.
-
Dietary consistency modification: The use of thick purees or high-cohesion foods facilitates bolus control and reduces the risk of premature spillage into the pharynx.
-
Use of specialized utensils: In some cases, small spoons or portion-control devices can improve safety during intake.
-
Patient and caregiver education: It is essential to ensure that the learned strategies are applied at home and in the patient’s daily environment.
Importance of a multidisciplinary approach
The management of propulsive oral stage dysphagia requires coordinated intervention from multiple professionals: speech-language pathologist, speech therapist, nutritionist, neurologist, and, in some cases, dentist or maxillofacial surgeon. This collaboration allows not only the symptoms to be addressed, but also the underlying causes and associated risk factors.
Prevention and follow-up
Although the onset of dysphagia cannot always be prevented, its progression can be delayed or its consequences minimized through regular assessments and maintenance exercises, particularly in patients with progressive diseases. Periodic follow-up, especially in older adults or individuals with neurological history, is essential for early detection of signs of propulsive oral stage dysphagia.
Conclusion
Propulsive oral stage dysphagia is a specific disorder within the broad spectrum of swallowing impairments. Although it often goes unnoticed, it can lead to serious consequences if not identified and treated in a timely manner. Its diagnosis requires careful assessment of lingual movements and oral bolus control, and its management should focus on strengthening the involved musculature and adopting strategies that promote safe and efficient swallowing.
Recognizing and managing propulsive oral stage dysphagia is key to maintaining the patient’s quality of life, preventing respiratory complications, and ensuring adequate nutrition. Timely and specialized care can make the difference between unsafe feeding and a functional swallowing process.
If you would like more information about NeuroAiD II, please fill out this contact form.
"*" indicates required fields


